5 mins read
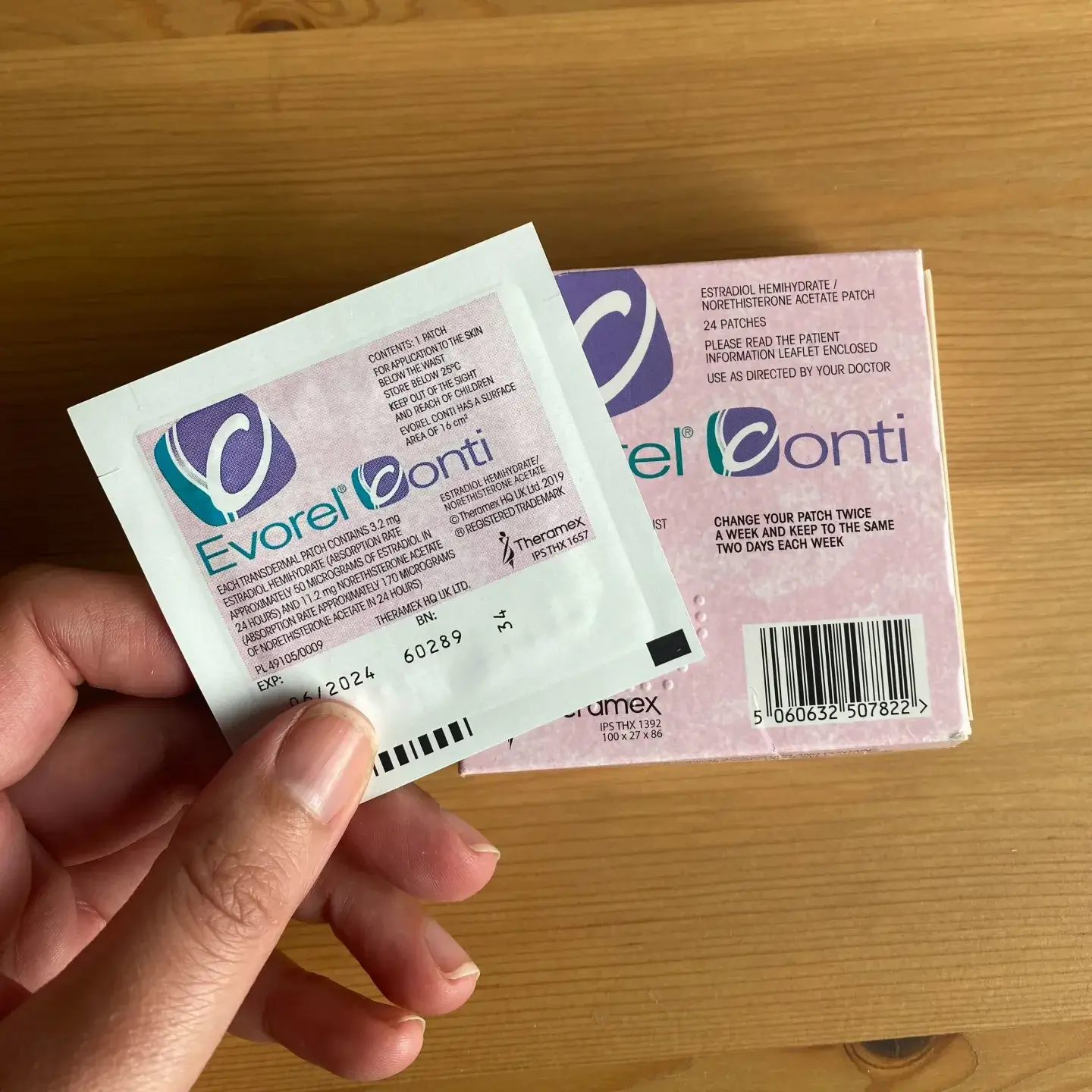
The Truth About Hormone Replacement Therapy
Talking recently with a group of female friends, I was surprised to hear that many still thought HRT was to be avoided and it wasn’t a good option to help with the symptoms of perimenopause.
And that got me thinking, with almost 50% of women experiencing emotional or physical symptoms of perimenopause, isn’t there a case for hormone replacement therapy in the 21st century? Why is HRT still so demonised and why are the benefits not being reliably communicated to women?
Menopause Impacting Women’s Quality Of Life
It can be difficult to understand just how the menopause can impact your quality of life if you haven’t yet experienced it.
In 2019, Forth published results from their survey involving 1,000 women and focusing on the impact the menopause has on their working lives.
It found that 63% of menopausal women felt their working life was negatively impacted by the menopause. Yet, for many women, there is an answer in the form of HRT.
So, why are only 17% of women aged between 40 and 65 using HRT to manage menopause symptoms?
The answer, in part, can be due to the press coverage of the risks of HRT that omit to also explain the benefits. Ask any woman about HRT and you are likely to hear their concerns about the increased risk of cancer and in particular breast cancer.

Why Did HRT Get A Bad Name?
The history of HRT treatment dates back to the 1960s with its popularity peaking in the late 1990s.
In the 1970s, the use of oestrogen supplements was associated with an increased risk of endometrial cancer which damaged the reputation of this previously popular menopause treatment.
In the years following, researchers found that reducing the amount of oestrogen and combining it with progesterone reduced the risk of endometrial cancer. So, this hormonal therapy was recommended for women who had not had a hysterectomy.
Whilst the Women’s Health Initiative Study 2002 reported an increased incidence of breast cancer with HRT, it transpired that the majority of recruits were 10 years past menopause and overweight at BMI 28. Being overweight is an independent risk factor for breast cancer.
In August 2019, the MHRA updated its guidelines on all forms of HRT following results published in The Lancet from a meta-analysis of 108,647 cases of breast cancer.
The study showed that approximately 1 in 16 women will be diagnosed with breast cancer between the ages of 50 and 69 who have never taken HRT for perimenopause or menopause.
Comparing this to women in their 40s and 50s who take oestrogen-only HRT for the menopause for 5 years, for every 200 women there would be one extra case of breast cancer:
- around 1 extra case per 200 women (corresponding to about 5 extra cases per 1000 women) who use oestrogen-only HRT
- around 1 extra case per 70 women (corresponding to about 14 extra cases per 1,000 women) who use oestrogen combined with progestogen for part of each month (sequential or cyclical HRT)
- around 1 extra case per 50 women (corresponding to about 20 extra cases per 1,000 women) who use oestrogen combined with daily progestogen HRT (continuous HRT)
However, the increased risk of breast cancer from HRT should be put in perspective. It is about the same increased risk as taking the combined oral contraceptive pill or drinking 2 or more units of alcohol per week, or smoking. This compares to a six-fold higher risk of breast cancer if you are overweight. So patient factors and lifestyle play a big part in breast cancer risk, independent of HRT.
The Case For HRT
In many cases, the benefits of taking HRT far outweigh the risks. A 2019 study found that women taking HRT close to their menopause had a lower risk of all-cause mortality including death related to cardiovascular disease.
In addition, NICE guidelines state that the risk of bone fractures is decreased in women taking HRT, and oestrogen-only HRT can help reduce the risk of developing heart disease.
This is because oestrogen plays a wide role throughout our bodies, from protecting our heart and bone health to boosting our immune system.
Oestrogen supports cardiovascular health by regulating the function of blood vessels as well as increasing HDL cholesterol and lowering LDL or bad cholesterol.
But that’s not all, oestrogen has also been shown to have an enhancing effect on the immune system through the regulation of specific immune cells.
The decreasing levels of oestrogen throughout the perimenopause means postmenopausal women are at an increased risk of autoimmune disorders, inflammation and are more susceptible to infections – in addition to an increased risk of osteoporosis and cardiovascular disease.
But it’s not just about improving longer-term health, HRT is taken by women as it dramatically improves their quality of life by reducing the distressing and debilitating symptoms of the perimenopause.
Summary
Fundamentally, whether or not to take HRT must be the choice of the individual, which means we need to be as informed as we can be to be able to make that choice when the time comes.
Each woman will go on her own journey towards menopause, experiencing different perimenopause symptoms to varying degrees. Some women will experience very few symptoms, while others will experience symptoms that impact their quality of life.
It is up to every woman to learn the facts about HRT and to decide if taking HRT is the right choice for her and her own set of circumstances.
This is exactly what I’ve done, and for me, HRT has been the right choice in managing my perimenopause symptoms and giving me back my quality of life.
Read Next: What Are The Benefits & Risks Of HRT?>>
- Health scores calculated
Close
Article references
-
Rymer, J., Brian, K and Regan, L. HRT and Breast Cancer Risk. BMJ: 367.
-
Cagnacci, A and Venier, M. (2019). The Controversial History of Hormone Replacement Therapy. Medicina (Kaunas): 55(9).
-
Ziel, H, K and Finkle, W, D. (1975). Increased Risk of Endometrial Carcinoma Among Users of Conjugated Estrogens. N Engl J Med: 293(23), pp 1167-70.
-
Murphy, E and Kelly, D, P. (2011). Estrogen Signaling and Cardiovascular Disease. Circulation Research: 109, pp 687-696.
-
Taneja, V. (2018). Sex Hormones Determine Immune Response. Front Immunol: 9.
-
Ghosh, M., Rodriguez-Garcia, M and Wira, C, R. (2014). The Immune System in Menopause: Pros and Cons of Hormone Therapy. J Steroid Biochem Mol Biol, pp 171-175.
-
Seeland, U et al. (2020). Evidence for Treatment with Estradiol for Women with SARS-CoV-2 Infection. BMC Medicine: 18.
This information has been medically written by Dr Thom Phillips
Thom works in NHS general practice and has a decade of experience working in both male and female elite sport. He has a background in exercise physiology and has published research into fatigue biomarkers.

Dr Thom Phillips
Head of Clinical Services
Related articles
Like this article? Here are some more based on similar topics.