
Female Hormone Imbalance Test
This single-day test gives a simple snapshot of your key female hormones along with thyroid function.
£89
6 mins read
Follicle stimulating hormone is an important sex hormone, in both men and women. Find out about its key roles in reproductive health and what it means if your levels are high or low.
Written by Leanne Edermaniger
August 6, 2024
Reviewed by:
Dr Thom PhillipsFollicle-stimulating hormone (FSH) is a hormone secreted by the anterior pituitary gland that has important roles in sexual health. It is a gonadotropic hormone that stimulates the growth and activity of the reproductive organs, ovaries in women and testes in men.
During the second and third trimesters of pregnancy, and the first three and six months after birth, the pituitary gland releases luteinising hormone (LH) and FSH. Both hormones peak during mid-pregnancy as the first ovarian follicle or seminiferous tubule matures in the developing foetus[1].
FSH levels remain low during childhood until puberty. During puberty, gonadotropin hormone-releasing hormone (GnRH) stimulates the secretion of LH and FSH from the anterior pituitary gland.
In boys, FSH and LH work simultaneously to stimulate the testes to produce testosterone, the hormone responsible for the development of male sex characteristics and sperm production.
In girls, FSH and LH stimulate oestrogen production from the ovaries. Oestrogen is one of the main female sex hormones and it encourages the development of female sex characteristics.
In women, FSH and LH control the menstrual cycle. The main role of FSH is to stimulate the development of ovarian follicles and prepare for ovulation.
Ovulation is a phase in the menstrual cycle which occurs around day 14 of a 28-day menstrual cycle. Ovulation is the release of an egg from the ovary.
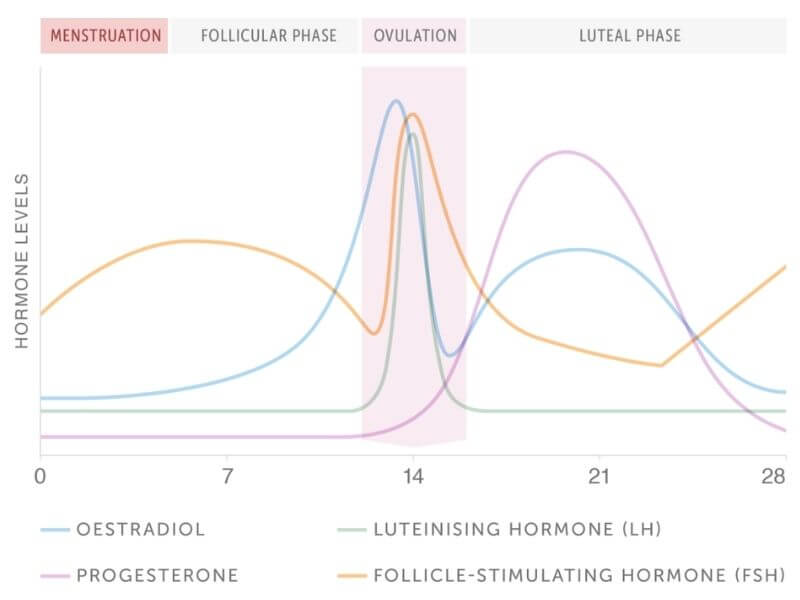
In the build-up to ovulation, around days six to 14, FSH levels increase and promote the development of ovarian follicles. During days 10 to 14, one of the ovarian follicles becomes dominant. A surge in LH around day 14 causes the dominant follicle to rupture and release the egg. This is ovulation.
Once ovulation has occurred, the ruptured follicle develops into a small ball of cells called the corpus luteum that produces a large amount of progesterone to prepare the womb for pregnancy and stop the production of FSH.
FSH levels then remain low throughout the luteal phase, stopping the development of new follicles, as the body prepares for potential pregnancy. If the egg isn’t fertilised, the corpus luteum breaks down, the menstrual cycle begins again, and FSH levels start to rise[2].
In women, FSH is critical in regulating the menstrual cycle, triggering the development of ovarian follicles and preparing the eggs for ovulation.
In men, FSH is important for normal sperm production[3].
Hormonal fluctuations in both men and women, including FSH, can have a detrimental impact on fertility.
According to the NHS, the normal reference ranges for FSH are:
| Adult male | 1.3 – 19.3 IU/L |
| Adult female during the follicular phase | 3.9 – 8.8 IU/L |
| Adult female mid-cycle | 4.5 – 22.5 IU/L |
| Adult females during the luteal phase | 1.8 – 5.1 IU/L |
| Peri- or postmenopausal | >16 IU/L[4] |
Data collected from Forth customers shows that FSH levels surge in women at peri- and postmenopausal age. Our results show a slight increase in male FSH levels in men over 60. This is consistent with other findings that state FSH (and LH) levels rise in men as testosterone levels fall[5].
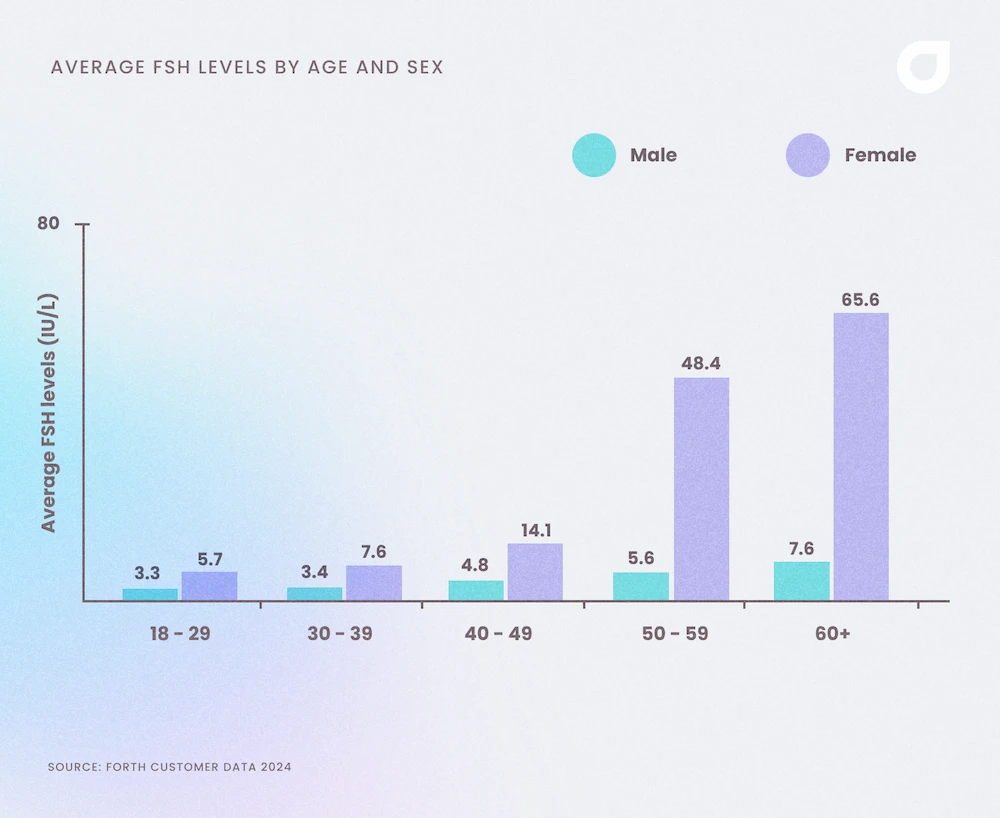
Forth data shows that the average FSH levels before menopause are 10.7 IU/L but rise to 60 IU/L after menopause. During menopause and postmenopause, FSH levels continue to increase because of the decline in oestrogen[6]. The low levels of oestrogen mean the feedback loop which tells the pituitary gland to stop producing FSH is disrupted, so FSH levels continue to rise[7].
| FSH Levels (IU/L) | |
| Before menopause | 10.7 |
| After menopause | 60.0 |
Several conditions can cause low FSH levels:
The symptoms of low FSH levels will depend on the underlying cause but may include:
Irregular periods
Impotence in men
Infertility
Low libido
Weight gain or loss[14]
High FSH levels are usually a side effect of hypogonadism – where the ovaries or testes produce no or low levels of hormones – causing the pituitary gland to release high levels of FSH as it tries to stimulate the gonads to produce more sex hormones.
Menopause
The natural decline in ovarian function during menopause leads to reduced oestrogen levels and increased FSH levels as the body tries to stimulate the ovaries to function normally.
Premature ovarian failure
Also known as primary ovarian insufficiency, premature ovarian failure is when a woman’s ovaries stop working before the age of 40.
Klinefelter syndrome
a genetic condition where boys are born with an extra X chromosome, causing testicular dysfunction and high FSH levels[15].
Turner syndrome
a genetic condition that affects females and is characterised by a missing or partially missing X chromosome. The condition causes elevated FSH levels[16].
Polycystic ovary syndrome (PCOS)
PCOS causes a rise in the LH: FSH ratio. It can also cause elevated FSH levels but is usually associated with high LH levels.
The symptoms of high FSH levels will often depend on the underlying cause. Here are some of the conditions associated with elevated levels and their symptoms:
| Condition | Symptoms |
| Menopause | Hot flashes, night sweats, vaginal dryness, mood swings |
| Premature ovarian failure | Similar to menopause and irregular periods |
| Klinefelter syndrome | Small testes, reduced muscle mass, breast development, infertility |
| Turner syndrome | Short, wide (webbed) neck, short stature, delayed puberty, infertility |
| PCOS | Irregular or no periods, difficulty getting pregnant, excessive hair growth, weight gain, acne |
You might be interested in checking your FSH levels if you are experiencing any symptoms associated with reproductive health or fertility.
Testing your FSH levels may help with:
Understanding why you’re experiencing irregular periods
Investigating fertility issues or why you might not be able to get pregnant
Confirming menopause
You can test your FSH levels with Forth using the following tests:
| MyFORM® Perimenopause Blood Test | Maps your hormones across your menstrual cycle to confirm perimenopause. |
| Female Fertility Blood Test | Gain a better understanding of your reproductive health if you are looking to try for a baby or are struggling to conceive. |
| MyFORM® Female Hormone Mapping | Track your hormone levels across your menstrual cycle to understand how well they function. Not for women currently taking hormonal contraception. |
| Female Hormone Imbalance Blood Test | This test checks your 4 key hormones; oestrogen, progesterone, LH, FSH and other key health biomarkers. It can help identify any imbalances and is suitable for women who currently use hormonal contraception. |
Other tests are available to check your FSH levels, such as over-the-counter menopause tests. These are often urine-based tests, similar to pregnancy tests, measuring the amount of FSH in urine. Because they only measure one hormone, FSH, these tests cannot accurately indicate whether a woman is in perimenopause or menopause[18].
Instead, tests like our MyFORM® Perimenopause Blood Test map all of the key female sex hormones across the menstrual cycle, providing a much more accurate insight into a woman’s fertility.
Based in the UK, Leanne specialises in writing about health, medicine, nutrition, and fitness.
She has over 5 years of experience in writing about health and lifestyle and has a BSc (hons) Biomedical Science and an MSc Science, Communication and Society.
All these tests include Follicle Stimulating Hormone (FSH). Select the test that suits your personal needs.
Certified for quality & security
Simoni, M., Weinbauer, G. F., Gromoll, J., & Nieschlag, E. (1999). Role of FSH in male gonadal function. Annales d'endocrinologie, 60(2), 102–106.
Mode of action of oral contraceptives. (1978). Family planning information service, 1(1), 11.
Thom works in NHS general practice and has a decade of experience working in both male and female elite sport. He has a background in exercise physiology and has published research into fatigue biomarkers.

Dr Thom Phillips
Chief Medical Officer