
Female Hormone Imbalance Test
This single-day test gives a simple snapshot of your key female hormones along with thyroid function.
£89
5 mins read
Sex hormone binding globulin (SHBG) is a protein that binds to and transports male and female sex hormones around the body. Changes in SHBG levels are linked to different conditions and symptoms in men and women
Written by Leanne Edermaniger
July 21, 2020
Reviewed by:
Dr Thom PhillipsSex hormone binding globulin (SHBG) is a protein made in the liver. It binds tightly to specific sex hormones, oestradiol, testosterone, and dihydrotestosterone (DHT), transporting them in their inactive forms in the blood. That means they cannot be used by your cells, it’s one of the ways the body regulates its hormone levels.
SHBG levels can change because of:
age
sex
chronic conditions
Testing SHBG levels can tell you how testosterone is working in your body. For example, high SHBG levels may mean there is less free testosterone available which can affect a man’s sex drive. While low levels mean more SHBG is available. In women, this can cause symptoms such as excess hair growth (hirsutism)[1].
The reference range for SHBG varies depending on the testing laboratory.
The normal reference range for the NHS is as follows:
| Gender | < 50 years old | > 50 years old |
| Male | 15 – 64 nmol/L | 14 – 78 nmol/L |
| Female | 19 – 145 nmol/L | 14 – 136 nmol/L[2] |
The healthy range for SHBG at our laboratory is:
| Men | 16.5 – 55.9 nmol/L |
| Women | 24.6 – 122 nmol/L |
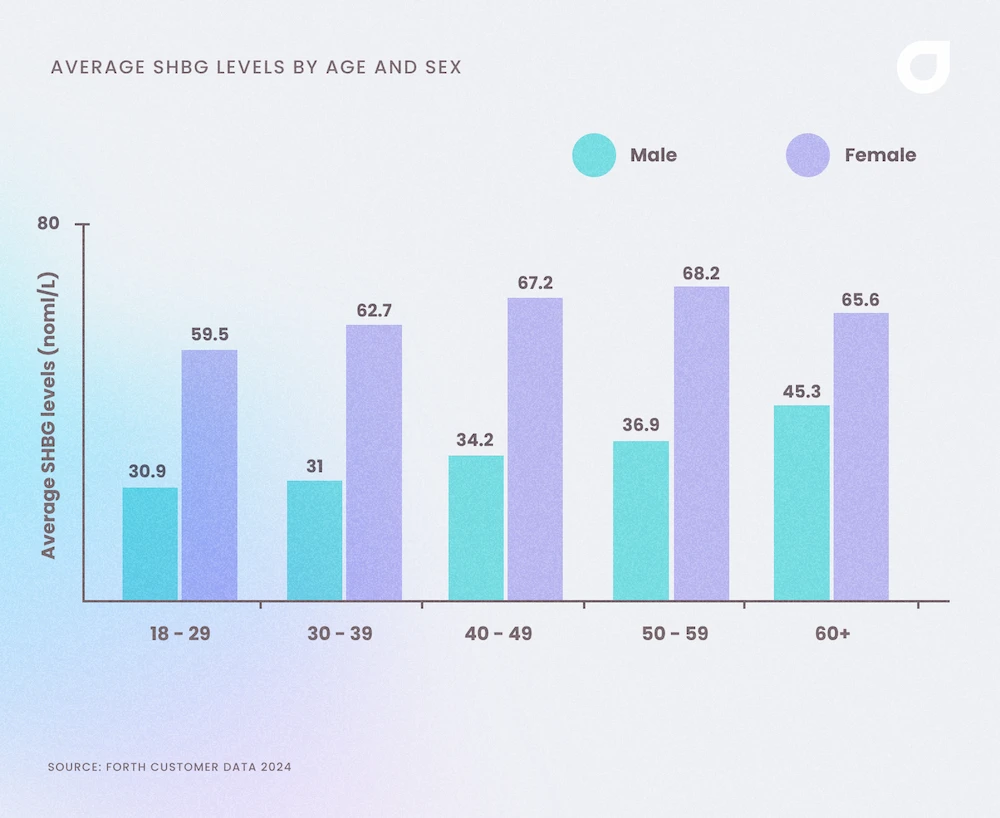
Forth data below shows the average SHBG level according to sex and age. For both sexes across all ages, SHBG levels are within the healthy range. However, SHBG levels typically rise in men as they get older because of declining testosterone which can be seen in the graph below.
If SHBG levels are low, it means there could be more sex hormones available for your body to use freely. The causes and symptoms of low SHBG can vary between men and women.
Low SHBG levels indicate a greater amount of free testosterone circulating in the blood. In women, high testosterone levels may be associated with polycystic ovary syndrome (PCOS).
PCOS is a common hormonal imbalance in women that can cause irregular periods and acne, and affect your chances of getting pregnant. It is associated with obesity and increases the risk of developing type 2 diabetes and heart disease[3].
Decreased SHBG levels in men and women are also linked to:
An underactive thyroid (hypothyroidism)
Obesity
High blood insulin (hyperinsulinemia)
Excess growth hormones
Family history of low SHBG[4]
Some research suggests that low SHBG levels may be related to some factors associated with the development of metabolic syndrome, like altered blood fat profiles, particularly in men[5].
In women, low SHBG levels are commonly associated with PCOS which can cause:
Acne
Weight gain
Hirsutism or excess facial and body hair
Mood swings
Hair loss on the head
Increased risk of cholesterol and type 2 diabetes
Difficulty conceiving
Irregular or absent periods[6]
PCOS affects 20% of women and causes psychological symptoms, like:
Reduced quality of life
Anxiety
Depression
Low self-esteem
In men, symptoms of low SHBG include:
Acne
Mood swings
Fluid retention
Liver disease
Weight gain
Increased muscle mass
Increased risk of blood clots
High blood pressure[7]
Metabolic syndrome is a group of health issues that increase the risk of developing type 2 diabetes and heart and circulatory conditions. Metabolic syndrome may not cause any symptoms but you could be at a greater risk if you:
are obese
are sedentary
smoke
eat an unhealthy diet
drink lots of alcohol
are Hispanic or South Asian[8]
Treatment for low SHBG levels will depend on the underlying cause. If you require medical treatment, your doctor will explain your results and the type of treatment you might need.
However, there are some things you can do to help raise your SHBG levels naturally.
Because low SHBG is predictive of metabolic syndrome, and is low in obese people, the effect of exercise on circulating SHBG has been researched.
A study involving 36 overweight, sedentary young men found that a 12-week resistance training program increased SHBG levels[9]. Another study involving obese postmenopausal women found that 16 weeks of aerobic exercise raised SHBG levels and could prevent obesity-induced metabolic syndrome[10].
The types of food you eat may be influencing your SHBG levels, particularly if you are overweight or obese. Research shows that a high sugar intake and consuming foods with a high glycaemic index (GI) were associated with lower levels of SHBG. Women who ate more dietary fibre, on the other hand, were more likely to have increased SHBG levels.
Examples of fibre-rich foods include:
Oats
Legumes (lentils, beans)
Fruit (apples, oranges, pears, cherries, berries)
Vegetables (sweet potato, spinach, peas, Brussels sprouts, broccoli)
Wholemeal or granary bread, wholewheat pasta, brown rice
Nuts (almonds, Brazil, cashews, pistachios)
High SHBG levels usually indicate a lower concentration of free sex hormones in circulation. There are a range of causes and symptoms linked to low SHBG levels.
If your SHBG levels are high it means your liver is overproducing the hormone. It can be a sign that your body is trying to correct imbalanced hormone levels or that your liver cells are not functioning as they should be.
Some of the common causes of high SHBG in men and women are:
Anorexia
Pregnancy (in women)
An overactive thyroid (hyperthyroidism)
Low testosterone levels
Low growth hormone levels
Liver disease
When SHBG levels are high, a higher proportion of sex hormones are bound and inactive. A short-term increase in SHBG levels can have protective benefits for the heart. However, high SHBG levels in the elderly aren’t desirable because they have been linked to an increased risk of fractures and weak bones[11].
In men, common symptoms of high SHBG levels are:
Erectile dysfunction
Low sex drive
However, symptoms can vary depending on the underlying cause of high SHBG levels. For example, common symptoms of hyperthyroidism are:
Mood swings
Weight gain
Anxiety
Irritability
Tiredness
Muscle weakness
Heat sensitivity
Sleep trouble
Thirst
Itchiness
Diarrhoea[12]
If an underlying medical condition is causing high SHBG levels, treating this may help to reduce them. There are certain lifestyle changes you can make to help reduce SHBG, including:
Diet changes
Eating a diet that is high in protein may help to lower SHBG levels, particularly in men. Protein-rich food include meat, fish, tofu, edamame, eggs, legumes, nuts and seeds.
Sex hormone binding globulin levels are measured as part of a wider hormone test, measuring the concentration of female and male sex hormones. It is usually carried out if you have any symptoms which may suggest high or low levels of testosterone.
You should test your SHBG levels if you are experiencing any of the symptoms listed above. The test will tell you how testosterone is working in your body.
In men, an SHBG test may cause symptoms associated with having too little testosterone, while women may be experiencing symptoms associated with too much. These can help to establish why you may be experiencing specific symptoms, and enable you to make certain lifestyle changes or receive medical treatment.
You can test your SHBG levels at home with one of the following Forth tests:
To get your results, simply:
Choose your test based on your requirements
Your kit will be sent to your address
Collect your sample by following the instructions enclosed in the kit
Post your sample back to the lab for analysis using the prepaid envelope
One of our GPs will review your results. You can access their comments on your secure health dashboard
Based in the UK, Leanne specialises in writing about health, medicine, nutrition, and fitness.
She has over 5 years of experience in writing about health and lifestyle and has a BSc (hons) Biomedical Science and an MSc Science, Communication and Society.
All these tests include Sex Hormone Binding Globulin (SHBG). Select the test that suits your personal needs.
Certified for quality & security
Thom works in NHS general practice and has a decade of experience working in both male and female elite sport. He has a background in exercise physiology and has published research into fatigue biomarkers.

Dr Thom Phillips
Chief Medical Officer