
Female health
13 mins read
Written by Jamie Braithwaite
September 14, 2022
Reviewed by:
Dr Thom Phillips
Periods are a natural process most women go through during their lives, with periods usually starting between the ages of 10-16 and carrying on until a woman reaches menopause at the average age of 51.
Although a natural process, periods can bring severe pain and discomfort that affect women in a range of ways, with common symptoms including; stomach aches, mood swings, a lack of energy and headaches.
Women’s experiences of periods will vary in terms of the symptoms suffered and the duration of their periods differing from person to person. However, a stigma still exists surrounding periods and discussing them openly, which, in turn, could harm women seeking assistance with their menstrual health.
Here at Forth, we wanted to explore women’s experiences with their periods in greater depth. Therefore, we conducted a survey of 1,000 women in the UK, aged 18 and over, who have periods, but are not on hormone birth control, HRT, or gel.
We did this to explore how comfortable women feel about discussing their periods, but also to explore the most common symptoms and attitudes towards periods within the workplace. The survey also included a quiz section to gauge how educated these women are on the effects of periods on the female body.
Firstly, the survey revealed that, on average, women say their period lasts 4.7 days.
The poll quizzed women on the extent of the pain suffered as a result of their periods. Only 5% stated they were not affected at all by period symptoms.
36% of women stated they find it uncomfortable to go to work and 30% responded that it makes working from home equally uncomfortable. Each month, 28% said they need to take a day off from work and 26% are unable to get out of bed.
70% of women revealed they get their period once a month. However, 19% stated their period was irregular, with 14% responding that theirs came every 2 months, while 6% experienced their period every fortnight.
The survey aimed to explore the most common symptoms for women suffering from their period but not on treatment. Our research revealed that stomach pain is the most frequently experienced, with 35% citing this symptom in the survey.
The top ten most commonly suffered symptoms were:

Of those suffering from stomach aches, 62% were of the 18-24 age range.
Interestingly, despite mood swings ranking as the second highest encountered symptom in the survey, only 10% of 51-55 year-olds revealed this as a common symptom.
The least commonly suffered symptoms include; greasy hair (14%), changes in sex drive (15%) and constipation (16%). 11% said they don’t have any symptoms.
The survey questioned women about who they feel comfortable enough with to discuss their periods and symptoms. The results revealed that 64% chose their partner as someone they can confide in, other responses include friends (47%) and family members (42%). 26% feel comfortable discussing their period with work colleagues.

Worryingly, only 19% stated they feel comfortable discussing their period with their GP, which can prove extremely damaging in ensuring women are receiving the help and advice needed to navigate symptoms and understand the changes in their bodies. West Midlands was the region with the lowest percentage of women feeling comfortable discussing their period with their GP, with only 9%.
28% of those living in South East said they would not feel comfortable speaking to anyone about their periods.
Regionally, 67% of Londoners have not sought advice from a GP, on the other hand, almost half (49%) of those surveyed from the East of England had got in touch with their doctor for advice.
Therefore, we explored the number of women who had sought advice from their GP. The results found that 52% of women had not gotten in contact with their doctor to seek advice on their symptoms. This reinforces the idea that women do not feel comfortable discussing this with medical professionals.
Of those who did visit their GP (32%), 63% felt their concerns were taken seriously and 62% believe they received the support needed to help manage symptoms. However, 30% felt they were not taken seriously and the same percentage (30%) said that they did not get the support they needed to help manage their symptoms.
65% of women who did visit their GP stated that they were offered hormonal contraception to assist with symptoms. Also, 69% shared that the doctor took a blood test in order to decide on how to manage period symptoms.
On the other hand, the survey respondents who didn’t feel comfortable talking with their GP revealed the reasons behind this. Those surveyed were allowed to select all that apply:
27% of women responded that they were unable to get an appointment with their doctor. This highlights the backlog still being felt as an aftereffect of the pandemic. When women decide to visit a GP, being knocked back with no appointment can be demotivating.
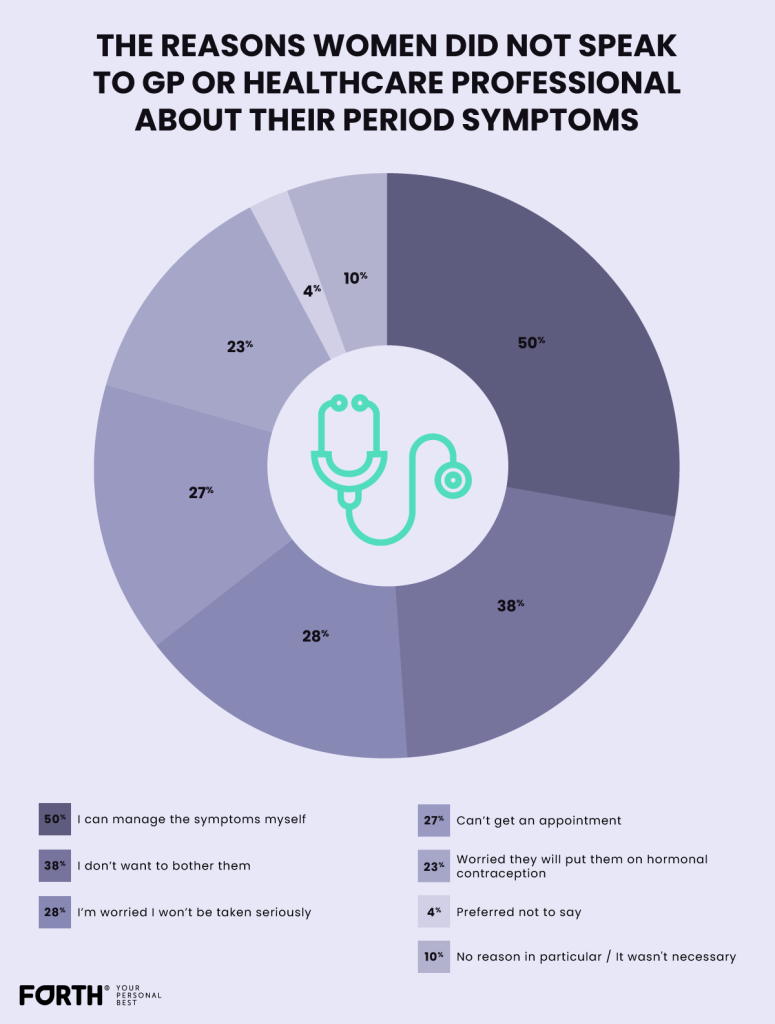
Of those who were unable to get an appointment with their doctor, 46% were from the East of England. On the other hand, only 9% of Northern Irish survey respondents claimed they struggled with getting an appointment.
Overall, we would advise any woman unsure of aspects surrounding their period to seek advice from a GP to ensure the best treatment is available should they need or want it in the future.
Another focus of our survey was to explore how women suffering from period symptoms and not receiving treatment manage at work.
With a previous survey question highlighting how uncomfortable symptoms can make women feel, it’s a useful insight to examine how much periods can affect day-to-day tasks such as employment.
Firstly, we asked how easy women find work when on their period. The results revealed that 30% believe it is neither easy nor difficult, whereas 16% find work fairly difficult and 6% very much so.
As a result, women have been forced to take days off work to recover from pain or discomfort felt from symptoms as a result of their periods.
We explored the number of days being missed as a result of these symptoms, the research found that 55% of the women surveyed have had to take time off work due to their period. Of this 55%, 15% took two days off and 20% were absent for three days as a result.
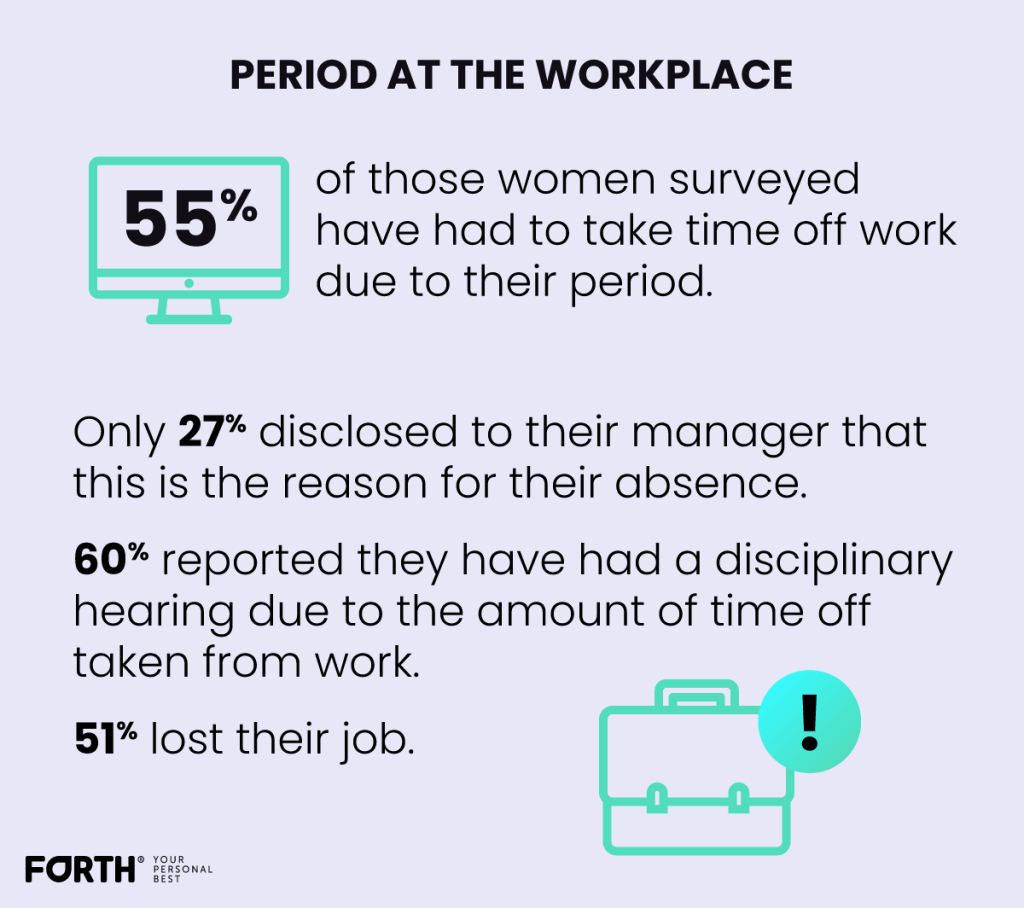
However, only 27% disclosed to their manager the reason for their absence. This validates that the stigma still exists surrounding periods in the workplace in the UK.
The research highlighted reasons why women did not tell their manager about their symptoms when requesting time off including:
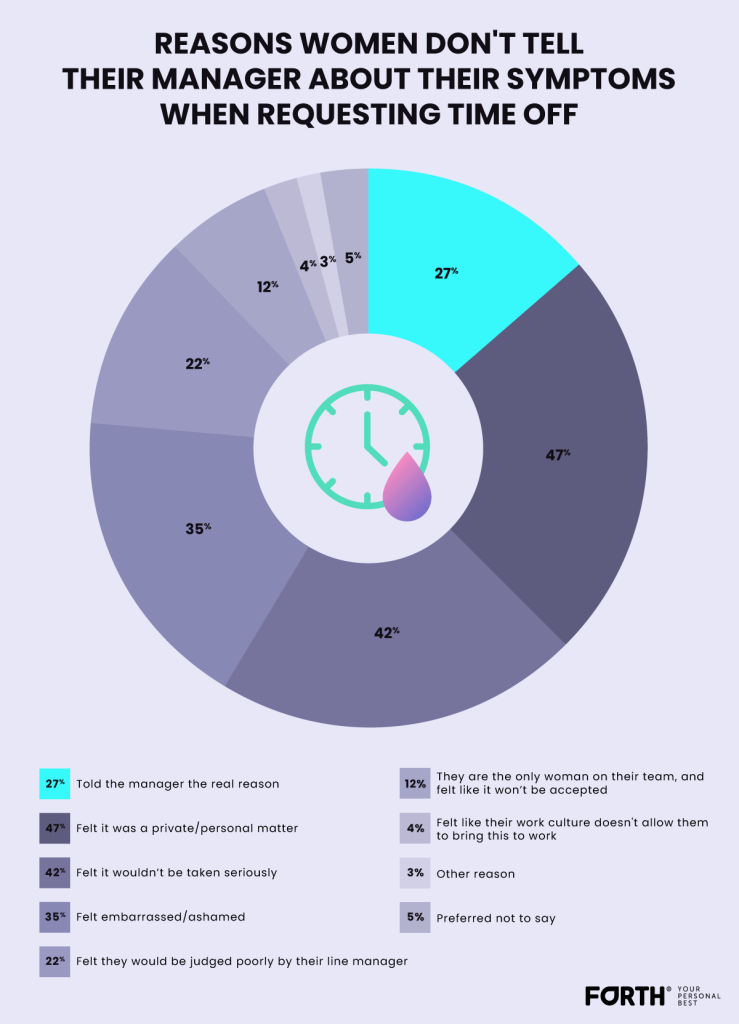
We believe more must be done to eradicate the stigma existing in the workplace to ensure women feel comfortable discussing their conditions.
Concerningly, 60% of those that did take a day off, reported they have had a disciplinary hearing due to the amount of time off taken from work. 51% of women who had been forced to take time off because of symptoms revealed they lost their job.
As periods are a natural occurrence in the female body, women should feel supported and have advice and treatment readily available to them should they desire it.
Sadly, this isn’t always the case, as we’ve already explored, with stigma seemingly existing throughout the workplace. Our survey explored this further, we quizzed women on whether they feel they have enough assistance.
Firstly, we asked survey participants how much support they believe is there for people suffering from symptoms of periods. A majority of 35% believe there is not enough support available and 19% responded that they were unsure.
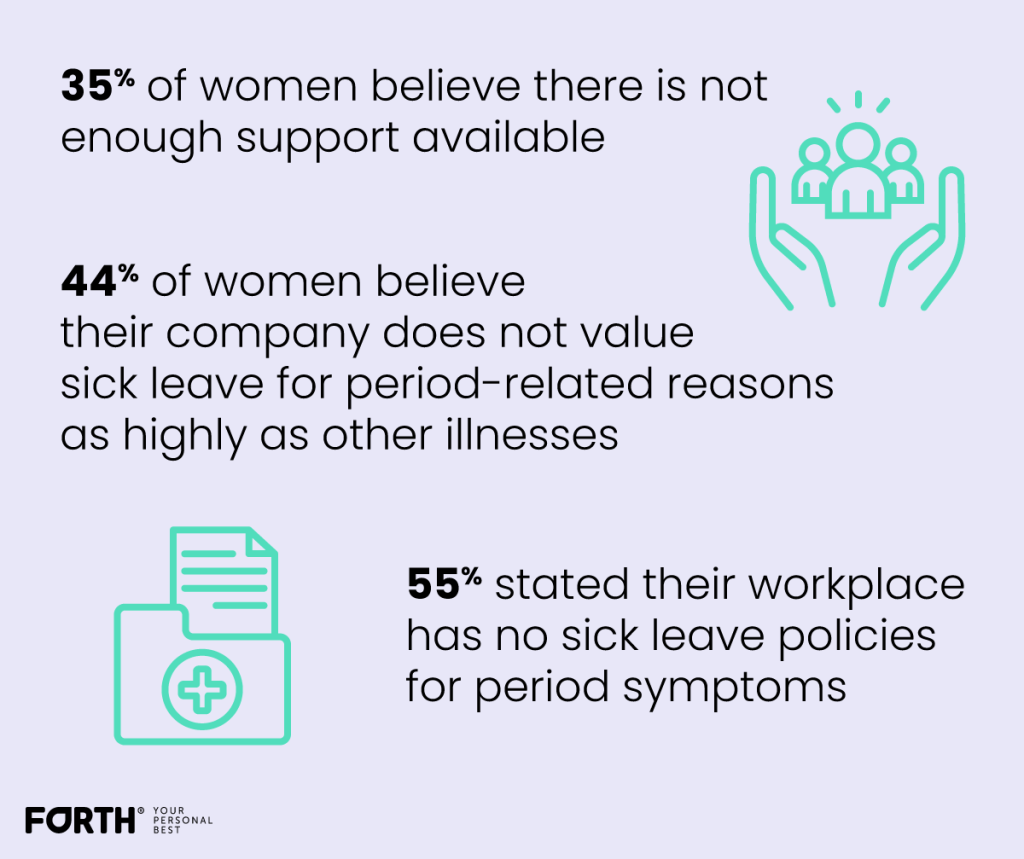
When it comes to the workplace, 44% of women believe their company does not value sick leave for period-related reasons as highly as other illnesses. On the other hand, 26% were unsure.
Over half of the respondents, 55%, also stated their workplace has no sick leave policies for period symptoms, highlighting a lack of support and empathy for women at work.
So now that it’s clear that women are suffering from symptoms related to their period, what support do they believe should be accessible?
Our survey asked respondents about the most important factors related to supporting women, they were allowed to select more than one response. The results were:
It was intriguing to see one-fifth of the women surveyed believe their GP should be better educated on how to approach and treat period symptoms.
This sentiment likely isn’t helped by a backlog of GP appointments, making actually seeing your GP a hurdle. This, combined with a lack of confidence discussing periods with GPs, has left traditional doctors appointments as unapproachable for a lot of women. That’s why we, at Forth, have put our expertise into at-home blood testing that empowers women to monitor their own hormone levels without even needing to leave their house.
Our MyFORM® hormone test is a blood test that can be utilised from the privacy of your home. The test measures hormone levels in the blood and allows women to visualise their fluctuating hormones to map their menstrual cycle and spot any irregularities.

It can also be used by older generations to spot peri or menopausal symptoms early and ensure women are aware of their bodily changes to seek any necessary treatment or advice.
Women can test themselves at home before sending off their blood to our female health experts but don’t worry, we won’t leave you waiting too long, as results are reported within 2 days of receiving your blood sample.
We believe that at-home testing is the future of female health, but our survey found that 61% of women have never completed a home blood test. Lack of general knowledge of at-home testing is potentially holding women back from the support they need, as our survey found that, of the 24% of women that had used home blood tests, a 66% majority found that the test aided in identifying the cause of period symptoms.
In the last section of our survey, we provided 1,000 adult women not taking hormonal birth control, HRT, or gel with general questions regarding periods to see how educated they were on hormones and their menstrual cycles.
Firstly, women were asked which statement best describes the definition of the menstrual cycle, they were given two choices:
The first statement was the correct definition, and 55% of women selected this option. Additionally, 21% were unsure, showing a potential need for improved education on basic women’s health, but the majority selected the correct definition of the menstrual cycle.
Next, the women surveyed were asked to select the hormones that are prominent in regulating the menstrual cycle. The correct options, progesterone and oestrogen were selected by the majority, with 28% selecting progesterone and 38% selecting oestrogen.
31% admitted they don’t know the answer.
Despite the majority selecting the correct answer to the first two questions, there is still a large portion of women who need further education on the hormones involved in the menstrual cycle.
The last question asked survey respondents to put the four stages of the menstrual cycle in the correct order. The correct order; menstruation, follicular phase, ovulation and the luteal phase were selected by only 16% of women surveyed.
48% of women responded with the four phases in the wrong order and 36% of those surveyed couldn’t provide an answer as they were unsure.
From the quiz section of the survey, it is clear that more must be done to ensure women are better educated on the science behind their menstrual cycle.
We hope this survey has provided valuable insight into a range of topics surrounding women and their periods – including support available, the stigma in the workplace, and the most common symptoms experienced.
With the use of demographic data, we are able to examine the regions and age range affected by certain factors, such as a lack of confidence in their GP.
Overall, we believe that more support needs to be made available for women suffering from intense symptoms. We also believe that by better-educating girls whilst in school and promoting discussion of periods, the stigma behind the natural occurrence can be diminished over time.
Disclaimer: One Poll surveyed 1,000 UK women aged 18 or over, who have periods and aren’t on hormonal birth control, HRT, or gel. The survey was conducted between the 18th and 24th of August 2022.
Thom works in NHS general practice and has a decade of experience working in both male and female elite sport. He has a background in exercise physiology and has published research into fatigue biomarkers.

Dr Thom Phillips
Chief Medical Officer