
Female Hormone Imbalance Test
This single-day test gives a simple snapshot of your key female hormones along with thyroid function.
£89
5 mins read
The free androgen index (FAI) estimates how much testosterone circulates in the blood. It is used to determine if a person has abnormal androgen levels, helping to diagnose conditions such as polycystic ovary syndrome (PCOS) in women.
Written by Leanne Edermaniger
July 25, 2024
Reviewed by:
Dr Thom PhillipsAndrogens are hormones that produce male characteristics, like facial hair and a deep voice[1]. The most common androgen is testosterone.
The free androgen index (FAI) measures how much biologically active or free testosterone is circulating in the blood. FAI can detect abnormal androgen levels, particularly in women.
Note: If you are on a high dose of biotin therapy (>5mg/day), you should collect your FAI test sample at least 8 hours after your last biotin dose.
A free androgen index test is recommended when an excess amount of androgens is suspected in the body. It most commonly affects women and causes symptoms, like facial hair growth (hirsutism) and irregular periods.
You can measure your free androgen index with a female hormone imbalance blood test or a polycystic ovarian syndrome (PCOS) blood test.
In men, low androgen levels can affect sex drive and are common in men with type 2 diabetes. Free androgen index in men is measured as part of our advanced and ultimate health checks.
The optimal free androgen index range for women is 0.19 to 3.63%. For men, it is 35 to 92.6%.
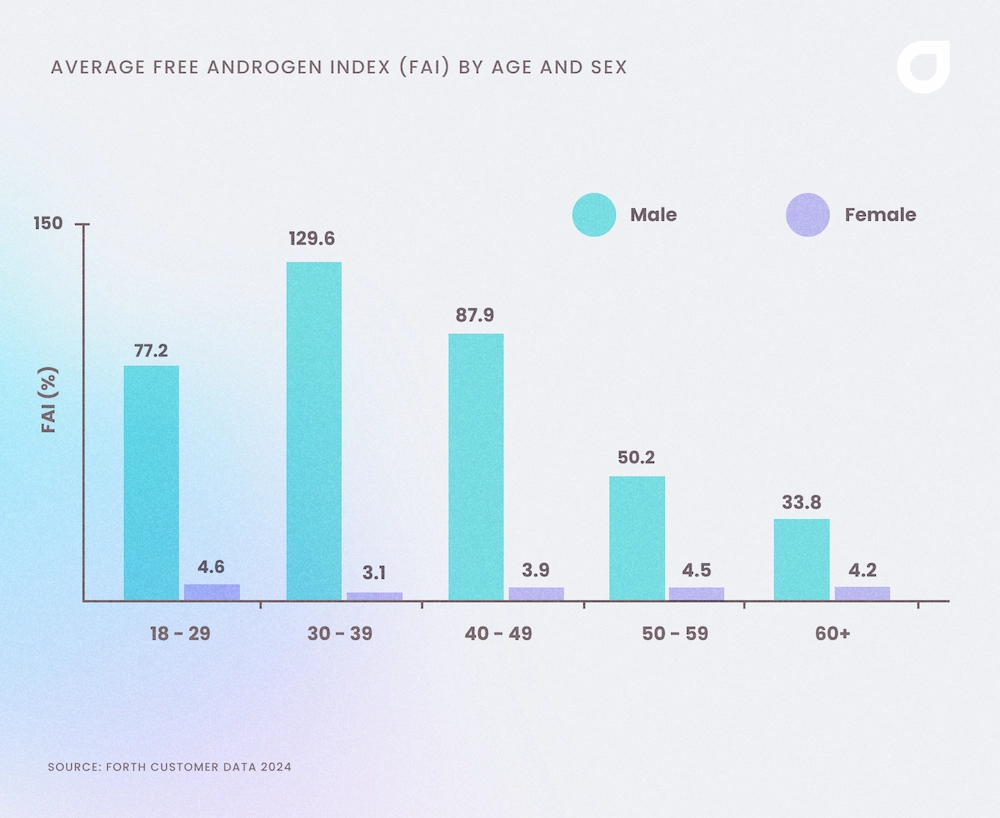
Data collected from Forth customers shows that the average FAI for women is 3.9% and 93% for men. The graph below shows the average FAI by age and sex.
The graph shows that the free androgen index peaks in men aged 30 to 39 before steadily declining.
The most common cause of high androgen levels in women is polycystic ovary syndrome (PCOS). PCOS affects approximately 10% of women[2] and is a condition that is characterised by an overproduction of testosterone by the ovaries. It can be distinguished by at least two of the following; high androgen levels, irregular periods, polycystic ovaries, or high anti-mullerian hormone (AMH) levels[3].
PCOS is associated with several other conditions, including:
Other causes of hyperandrogenism are:
Common symptoms of high androgen levels in women are:
Low testosterone or androgen levels are a common side effect of getting older in women. They naturally decline with age, some women may not notice the effects while others may be very sensitive to the change. Premenopausal women produce three times as much testosterone as oestrogen.
Other causes of low androgen levels in women include:
The most common androgen deficiency symptoms are:
It’s rare for androgen levels to become too high in men. Often the cause is medication or supplements, such as anabolic steroids.
Anabolic steroids are a synthetic version of the male hormone, testosterone and can have a powerful effect on the body like increasing muscle mass[11]. They are often used to enhance sports performance.
Certain cancers may also cause a rise in androgens, particularly testosterone. Recent research suggests that men with a higher level of free testosterone and a growth hormone called IGF-I were more likely to be diagnosed with prostate cancer[12]. Rarely, high androgen and oestrogen levels in men are associated with testicular cancer, more specifically Leydig cell tumours[13].
The effects of hyperandrogenism in men will depend on the cause. For example, if the adrenal glands cause excess hormones, there will be few side effects, but it can reduce the function of the testes and cause infertility.
If high androgen levels are caused by anabolic steroid use, the symptoms can include:
A low free androgen index in men below 35 can indicate testosterone deficiency. Age-associated testosterone deficiency syndrome, also known as late-onset hypogonadism, is a clinical condition that’s linked to increasing age. It is diagnosed when the blood testosterone level is below the reference range for young healthy adult males[15].
Interestingly, low testosterone levels are also commonly associated with type 2 diabetes[16]. Some research suggests that higher testosterone levels can reduce the risk of type 2 diabetes in men, so testosterone is a protective factor against metabolic disease[17].
Common symptoms of late-onset hypogonadism include:
Although little scientific evidence supports the claims, several foods have been suggested to help lower testosterone levels in women. They include:
Some research has reported a significant benefit of vitamin D supplementation on male hormone concentrations[22]. A study published in 2021 found that vitamin D supplementation lowers hirsutism scores and androgen levels in overweight women with PCOS[23].
Our data shows that 57% of UK adults are deficient in vitamin D. The NHS recommends that all UK adults consider a daily 10 microgram (mcg) vitamin D supplement during autumn and winter because the sun is not strong enough for the body to make it[24].
Based in the UK, Leanne specialises in writing about health, medicine, nutrition, and fitness.
She has over 5 years of experience in writing about health and lifestyle and has a BSc (hons) Biomedical Science and an MSc Science, Communication and Society.
All these tests include Free Androgen Index. Select the test that suits your personal needs.
Certified for quality & security
‘International evidence-based guideline for the assessment and management of polycystic ovary syndrome – 2023’ (2023) REPRODUCTIVE ENDOCRINOLOGY, (69), pp. 59–79. doi:10.18370/2309-4117.2023.69.59-79.
Mazer N. A. (2002). Testosterone deficiency in women: etiologies, diagnosis, and emerging treatments. International journal of fertility and women's medicine, 47(2), 77–86.
Jakiel, G., & Baran, A. (2005). Hipoandrogenizm u kobiet [Androgen deficiency in women]. Endokrynologia Polska, 56(6), 1016–1020.
Yao, Q. et al. (2018) ‘Testosterone level and risk of type 2 diabetes in men: A systematic review and meta-analysis’, Endocrine Connections, 7(1), pp. 220–231. doi:10.1530/ec-17-0253.
Mínguez-Alarcón, L. et al. (2017) ‘Fatty acid intake in relation to reproductive hormones and testicular volume among Young Healthy Men’, Asian Journal of Andrology, 19(2), p. 184. doi:10.4103/1008-682x.190323.
Thom works in NHS general practice and has a decade of experience working in both male and female elite sport. He has a background in exercise physiology and has published research into fatigue biomarkers.

Dr Thom Phillips
Chief Medical Officer