Breakthrough test

MyFORM® Perimenopause Test
Understand if symptoms you're experiencing could be due to perimenopause with our ground-breaking hormone mapping test.
£129
8 mins read
For many, the menstrual cycle can feel like a hormonal minefield, but understanding yours is key to understanding you, identifying patterns, and ultimately proactively taking charge of your health. Here, we’ll break down the menstrual cycle into its basics, uncover the mystery surrounding hormones, and equip you with the tools you need to confidently track your cycle, so you can spot what’s ‘normal’ for you.
Written by Leanne Edermaniger
January 24, 2025
Reviewed by:
Dr Thom Phillips
A menstrual cycle is a monthly series of changes that a woman’s body undergoes to prepare for pregnancy. Controlled by your hormones, a cycle begins on the first day of your period and ends when your next period begins. The length of your cycle is individual to you and can last anywhere between 21 and 35 days, although on average it lasts about 28 days.
A menstrual cycle consists of four main phases which we’ll cover in more detail later, but they are:
Periods begin when your body is ready, which can be anywhere between the ages of 8 and 17 years old. In the UK, the average age a girl starts her menstrual cycle is 12 years old[1].
Most women will get a monthly period until menopause. In the UK, perimenopause and menopause usually occur between the ages of 45 and 55 years old, with the average age of menopause being 51.
However, every woman’s experience will be different and unique to them, so don’t worry if you don’t quite fit into these averages.
The average length of a menstrual cycle is 28 days but it can be as short as 21 days or as long as 35 days[2], it really depends on your body.
The first day of your cycle is the day you get your period. A period usually lasts 2 to 7 days and consists of blood and your womb lining. Although it may look like a lot of blood, women usually lose around 20 to 90 millilitres of blood during each period. Some women may experience heavier periods and may require some help with dealing with them.
Usually, you’ll start to notice the signs a period is coming on in the days before it happens. Premenstrual syndrome (PMS) occurs when the hormones in control of your menstrual cycle change, affecting your emotions and well-being. PMS symptoms include:
Sometimes your periods can change, so you’ll need to keep a lookout for anything out of the ordinary. You might experience heavier or lighter periods or they may become longer or shorter. This doesn’t always mean there is an issue, but if you notice any changes you should speak to your doctor or nurse to investigate the cause.
Your hormones are critical for controlling the menstrual cycle and there are four key hormones involved:
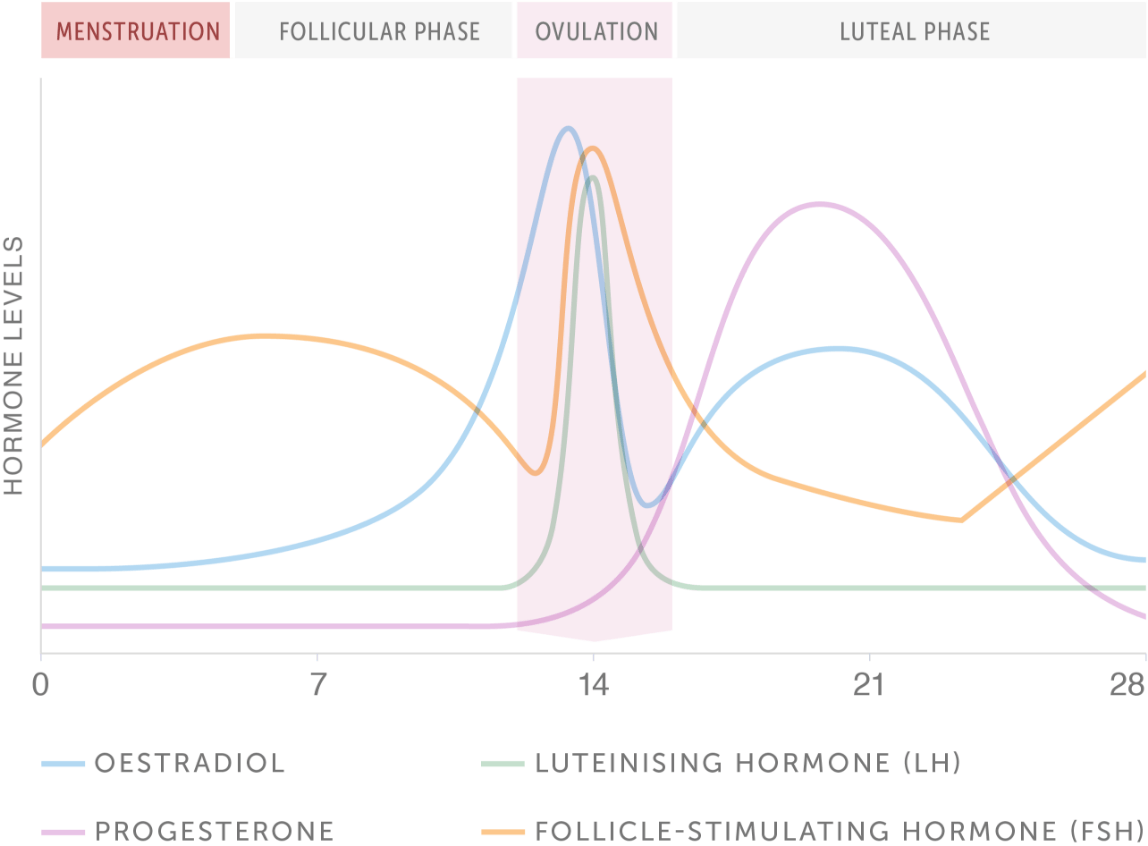
The menstrual cycle is split into four distinct phases.
The first stage of the menstrual cycle is the menstrual phase or menstruation and is when you get your period.
Your period usually spans days one to five and happens because an egg from the previous cycle hasn’t been fertilised, so there’s no pregnancy for the body to prepare for. Oestrogen and progesterone levels fall, causing the lining of the uterus, which thickened to support pregnancy, to be shed through the vagina. During your periods, you’ll release a mixture of uterine tissue, blood, and mucus.
The follicular or proliferative phase of the menstrual cycle is when ovarian follicles start to mature in preparation for releasing an egg during ovulation. This phase starts on day one of your period, so there is some overlap with the menstrual phase, and ends when you ovulate.
During the follicular phase, your pituitary gland releases follicle-stimulating hormone (FSH), stimulating your ovaries to produce follicles, fluid-filled sacs that contain immature eggs.
Normally, one egg, often the healthiest one, will fully mature, setting off a surge in oestrogen, causing the womb lining to thicken in preparation for a fertilised egg to implant itself and grow. On average, the follicular phase lasts around 15 days but this may be shorter or longer depending on your cycle pattern[4].
Increasing oestrogen levels during the follicular phase stimulates the release of luteinising hormone (LH). This kicks off the ovulation phase of your cycle.
Ovulation is when a mature egg is released from your ovaries. The egg travels down the fallopian tubes to the uterus where, if it meets sperm, it can be fertilised. Hence, the ovulation period is when pregnancy is possible.
Ovulation is the midpoint of your cycle, usually occurring on or around day 14 of your cycle.
The luteal phase occurs from days 14 to 28 of the menstrual cycle. Once an egg has been released, the follicle transforms into a structure called the corpus luteum which releases progesterone and some oestrogen to keep the body prepared for pregnancy.
If an egg isn’t fertilised, the corpus luteum eventually shrinks away, resulting in a drop in oestrogen and progesterone, causing your period to start again.
If you do become pregnant, the corpus luteum continues producing progesterone to maintain the womb lining. Your body will also produce human chorionic gonadotropin (hCG), the hormone that’s detected by pregnancy tests to give you a positive result.
If you want to become pregnant, the best time to try for a baby is the five days leading up to ovulation, the day of ovulation, and the day after ovulation. This is known as your fertility window and is when you are most likely to get pregnant.
Sperm can survive for 5 to 7 days inside your body, so it is possible to become pregnant if you have sex in the days leading up to ovulation. Tracking your menstrual cycle with MyFORM can help you gain a better understanding of when you will ovulate, so you can plan when to have sex for the best chances of conceiving.
Several factors can influence your menstrual cycle, including:
Menstrual symptoms can vary between women with some experiencing mild discomfort while others may report more intense or severe effects. Some of the common period symptoms include:
Premenstrual symptoms occur because of the hormonal fluctuations that take place during your cycle. For example, a rapid drop in oestrogen and progesterone levels in the run-up to you getting your period can cause many of the physical and emotional changes you might experience.
Don’t worry, you’re not alone, just 5% of women told us they are not affected by period-related symptoms at all!
There are some things you can do to help manage your symptoms, like:
Tracking your menstrual cycle is one of the best ways to identify patterns in your cycle. You can do this in various ways, including:
Tracking your menstrual cycle can help you:
Understanding your menstrual cycle gives you a clear insight into how your hormones are changing and affecting you on a monthly basis. The MyForm blood test provides you with a more accurate picture of your menstrual cycle, enabling you to track hormonal fluctuations that are important for predicting when you’ll get your next period, the best time to get pregnant, and link any patterns or symptoms to rising or falling hormone levels.

Our ground-breaking perimenopause blood test uses 2 blood samples to map your hormones across your entire menstrual cycle, showing the hormone patterns associated with perimenopause and giving you a clearer picture of your ovarian response.
Breakthrough test

Understand if symptoms you're experiencing could be due to perimenopause with our ground-breaking hormone mapping test.
£129
Bull, J.R. et al. (2019) ‘Real-world menstrual cycle characteristics of more than 600,000 menstrual cycles’, npj Digital Medicine, 2(1). doi:10.1038/s41746-019-0152-7.
Thom works in NHS general practice and has a decade of experience working in both male and female elite sport. He has a background in exercise physiology and has published research into fatigue biomarkers.

Dr Thom Phillips
Chief Medical Officer
Like this article? Here are some more based on similar topics.