
Female Hormone Imbalance Test
This single-day test gives a simple snapshot of your key female hormones along with thyroid function.
£89
4 mins read
Your pituitary gland makes luteinising hormone, important for regulating your reproductive health. Fluctuations in LH levels can impact your sexual health and fertility in several ways.
Written by Leanne Edermaniger
August 16, 2024
Reviewed by:
Dr Thom PhillipsLuteinising hormone (LH) is a gonadotropic hormone produced and released by the anterior pituitary gland. It has important roles in men’s and women’s sexual health and function.
LH works alongside follicle-stimulating hormone (FSH) signalling to the sexual organs (testes or ovaries) to initiate the processes required to support your reproductive health:
In men, LH stimulates the testes to make testosterone, a male sex hormone that’s essential for sperm production.
In women, LH is important during the second half of the menstrual cycle, preparing the body for pregnancy.
In menstruating women, LH helps regulate the menstrual cycle. During the first two weeks of the cycle, LH, alongside FSH, stimulates ovarian follicles to produce a type of oestrogen called oestradiol. Once a critical level of oestradiol is achieved, LH levels surge around Day 14 of the menstrual cycle, initiating the release of an egg from the ovary (ovulation)[1].
Once ovulation has occurred, LH then acts on the corpus luteum, the collection of cells from which the egg was released, to release more progesterone. Progesterone supports the early stages of pregnancy if fertilisation happens. If it doesn’t hormone levels fall and the cycle begins again[2].
During perimenopause, ovarian function declines, causing hormonal fluctuations. Specifically, LH levels can be erratic across the cycle, leading to irregularity and contributing to the development of perimenopausal symptoms.
High LH levels are also a sign of reduced ovarian reserve and function, meaning a woman is transitioning towards menopause.
Luteinising hormone is important in both male and female fertility:
Oocyte development
The mid-cycle surge in LH, ensures the ovarian follicles mature and that an egg is ready to be released[3].
Hormone regulation
LH is critical for ovulation in women and for the production of testosterone in men which is essential for sperm production.
Spermatogenesis
In men, LH stimulates the Leydig cells in the testes to make testosterone. In combination with FSH, LH initiates and maintains the normal production of sperm (spermatogenesis)[4].
When analysing luteinising hormone levels and considering what values are normal, many factors must be taken into consideration, like:
Age
Sex
Where you are in your menstrual cycle
If you have been through menopause
LH levels of menstruating women fluctuate during their cycle, surging around Day 14. While perimenopausal, menopausal, or postmenopausal women are likely to see rises in their levels as ovarian function and oestrogen production declines.
The normal range for LH can also be different between laboratories. The normal LH ranges for our labs are:
| Pre-menopausal women | 2.4 – 12.6 IU/L |
| Post-menopausal women | 7.7 – 59 IU/L |
| Men | 1.7 – 8.6 IU/L |
During the follicular and luteal phase of the menstrual cycle, LH levels are relatively low, the surge mid-cycle can cause a large increase and signifies when a woman is most likely to become pregnant. However, after menopause, LH levels remain high. We can see this in the data collected from Forth customers:
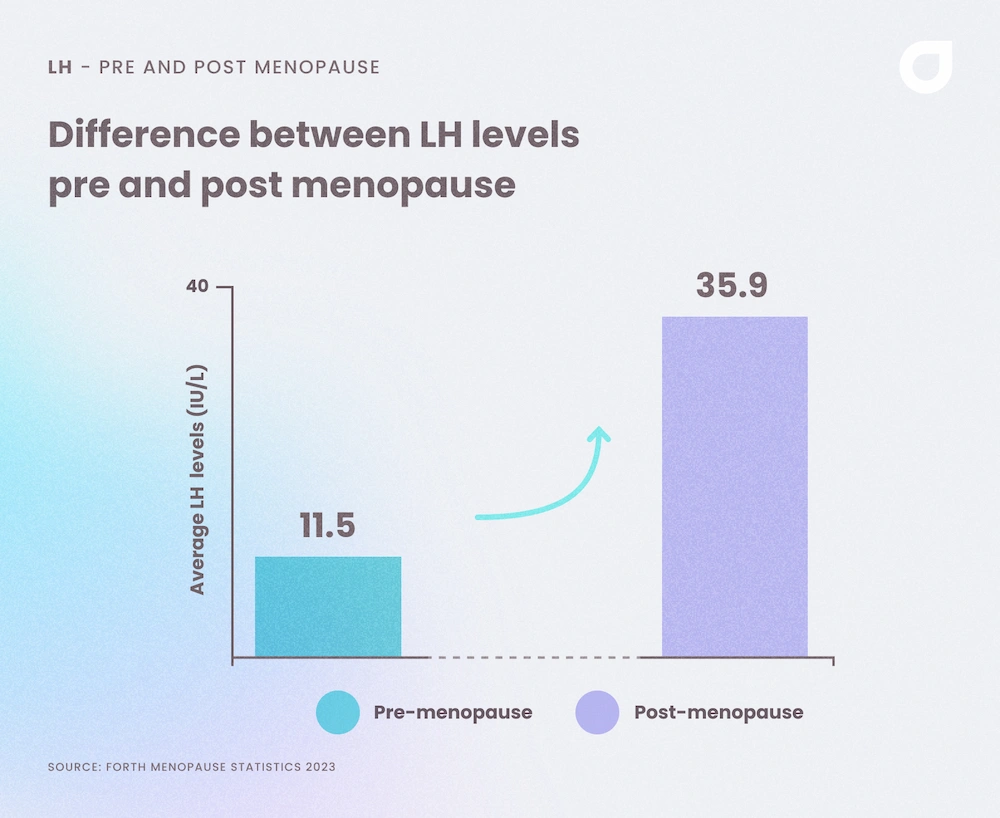
It’s also possible to see a steady increase in LH levels throughout a woman’s life, using data collected from Forth customers. The graph also shows that LH levels remain relatively constant in men.
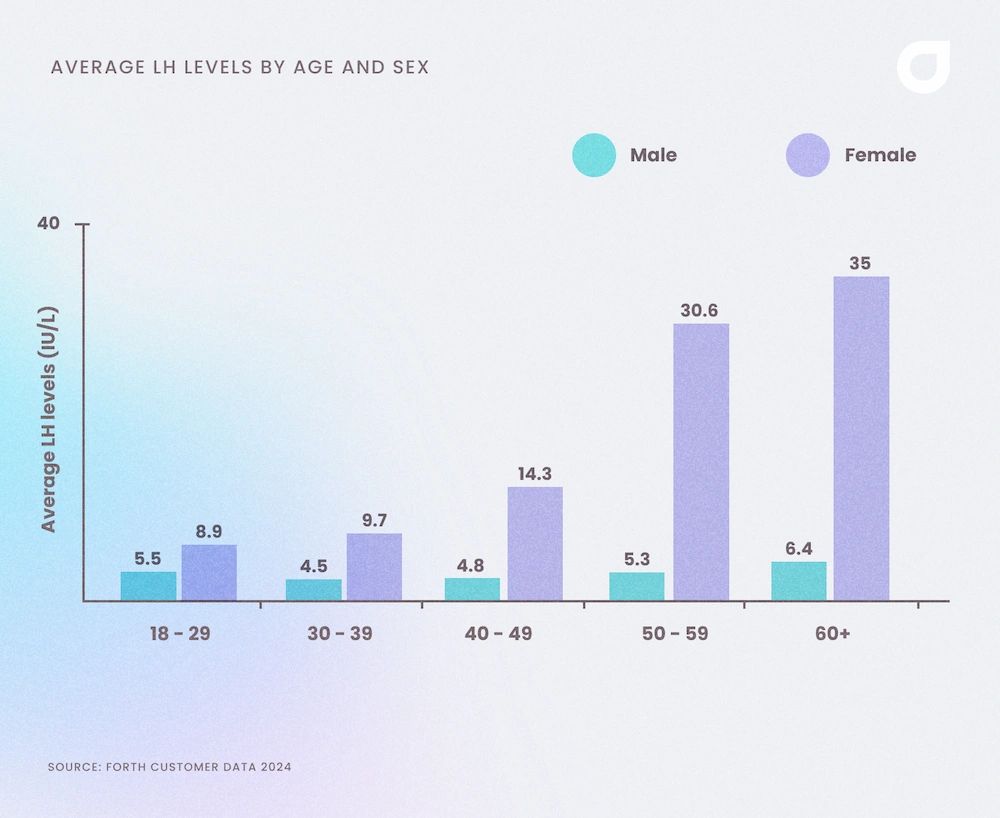
LH levels naturally fluctuate, particularly during the menstrual cycle, so high or low levels aren’t always a good or bad sign. A surge in LH midway through your cycle could suggest you’re about to ovulate and could be beneficial if you are planning a pregnancy.
That’s why it is important to consider factors like your age and menstruation status when assessing LH levels.
High luteinising hormone levels can be a sign that your sexual organs aren’t producing enough hormones required to regulate reproductive processes in the body. Some of the causes include:
Turner syndrome
affects females and is caused by a full or partial deletion of an X chromosome. The condition impairs ovarian function and a rise in LH as it tries to stimulate the ovaries to work[5].
Klinefelter syndrome
affects males only and is caused by carrying an extra X chromosome. It causes small testes that do not produce enough testosterone to support sperm production.
PCOS
Polycystic ovary syndrome (PCOS) is a common condition that affects how a woman’s ovaries work, causing irregular periods, high levels of male hormones, and cysts to develop on the ovaries. The condition causes debilitating symptoms and may affect fertility. Although the cause is unknown, hormonal imbalances are common in PCOS, including high levels of testosterone, LH, and prolactin, and low levels of sex hormone-binding globulin (SHBG)[6].
Menopause
The decline in ovarian function, causes elevated LH levels as the hormone tries to stimulate the ovaries to produce oestrogen and work normally.
Low levels of luteinising hormone can be a sign that the pituitary gland isn’t making a normal amount of LH.
Low LH levels may be caused by:
Kallman syndrome
an inherited condition resulting in a lack of gonadotropin-releasing hormone (GnRH) being released by the hypothalamus, causing low FSH and LH levels. The condition only affects men and boys.
Functional Hypothalamic Amenorrhoea
an absence of periods in girls and women often caused by psychological stress, excessive exercise, or weight loss. It causes a low production of GnRH, resulting in low LH levels[7].
Luteinising hormone is usually requested by a doctor when a couple is finding it difficult to conceive. It’s measured using a blood sample taken from a vein in your arm.
However, you can also test your LH levels at home. The following Forth tests measure your LH levels:
Measuring your LH levels at a specific moment in time can help you understand:
If a pituitary gland or hypothalamic disorder is causing LH fluctuations
What might be causing fertility problems
Why you might be experiencing irregular or absent periods
If you are transitioning through menopause
Why you might have low testosterone levels
If your LH levels or high or low and are causing symptoms or they are affecting your quality of life, you should consult your doctor for advice and treatment.
However, there are things you can do to support your LH levels and help to keep them within a healthy range. Generally, you can support your reproductive function by:
Eating a healthy, balanced diet incorporating lots of fruit, vegetables and wholegrains, and choosing lean cuts of meat over fatty or processed options.
Getting regular exercise. Most adults should aim to complete 150 minutes of physical activity per week. Exercise is good for both your physical and mental health.
Quitting smoking and lowering your alcohol intake.
Getting a good night’s sleep can help to promote proper hormone regulation.
If your LH levels are raised, you may find it helpful to:
Quit smoking
Some research shows that smokers tend to have higher LH levels at the time of their period compared to non-smokers. This may impact the fertility and reproductive health of smokers[8]. If you are trying to conceive and you smoke, it is recommended to quit smoking to help improve your chances of conceiving and preventing any damaging effects.
Lower your alcohol intake
Some evidence suggests that regular alcohol consumption can increase LH levels. Cutting down on your alcohol intake may help to normalise your levels.
Try hormone replacement therapy (HRT) if you are menopausal
The rapid decline in oestrogen production in menopause can cause several debilitating symptoms, most notably hot flashes, night sweats, mood swings, and vaginal dryness. It also causes raised LH levels. Some women find HRT is an effective way to manage their symptoms and studies show it can help reduce LH and FSH levels[9].
Some lifestyle factors can influence your LH levels. Relative energy deficiency in sport (RED-S) is a condition caused by an imbalance in energy intake and energy expenditure. For example, a low caloric intake paired with an increased level of exercise which means you do not have enough energy to adequately fuel the body during physical activity.
RED-S can affect men and women, resulting in hormone imbalances, including low LH levels, and causing a myriad of symptoms, and even contributing to infertility[10]. Therefore, it is important to evaluate your diet and exercise regime to ensure you are adequately fueling your body.
Based in the UK, Leanne specialises in writing about health, medicine, nutrition, and fitness.
She has over 5 years of experience in writing about health and lifestyle and has a BSc (hons) Biomedical Science and an MSc Science, Communication and Society.
All these tests include Luteinising Hormone (LH). Select the test that suits your personal needs.
Certified for quality & security
Castelo-Branco, C., Martínez de Osaba, M. J., Fortuny, A., Iglesias, X., & González-Merlo, J. (1995). Circulating hormone levels in menopausal women receiving different hormone replacement therapy regimens. A comparison. The Journal of reproductive medicine, 40(8), 556–560.
Todd, E., Elliott, N. and Keay, N. (2022) ‘Relative energy deficiency in sport (red-S)’, British Journal of General Practice, 72(719), pp. 295–297. doi:10.3399/bjgp22x719777.
Thom works in NHS general practice and has a decade of experience working in both male and female elite sport. He has a background in exercise physiology and has published research into fatigue biomarkers.

Dr Thom Phillips
Chief Medical Officer