
Female Hormone Imbalance Test
This single-day test gives a simple snapshot of your key female hormones along with thyroid function.
£89
8 mins read
Oestrogen is one of the main female sex hormones, but it is important for regulating mood, bone density, heart health and libido in both sexes. Find out what an oestrogen imbalance can mean for you.
Written by Leanne Edermaniger
July 26, 2024
Oestrogen is one of the main female sex hormones. Although both men and women produce oestrogen, it is important for the development of female sex characteristics during puberty, regulating the menstrual cycle, and promoting bone health.
Women produce three types of oestrogen across their lifetime:
Oestrone is made in adipose tissue and has a major role after menopause.
Oestradiol is the most powerful type during the perimenopausal period and is responsible for regulating the menstrual cycle.
Oestriol is the least potent form of oestrogen which is important during pregnancy and is produced in large amounts by the placenta.
Oestradiol is mostly secreted by the ovaries in women but can also be produced by the adrenal glands in both sexes and the testes in men.
Oestrogen has crucial roles in female sexual and reproductive health.
Oestrogen has effects on many different areas of the body, including:
Menstrual cycle regulation: Alongside progesterone, oestrogen regulates the menstrual cycle, peaking around 2 weeks before a period. It then rises again during the second phase of the cycle.
Oestrogen levels naturally decline with age. They tend to peak during the mid to late 20s in women and reduce by 50% by age 50, before dramatically falling after menopause[4]. The rapid decline in oestrogen is associated with many menopause symptoms, like hot flashes, night sweats, and vaginal dryness. This can lead to some women opting to take oestrogen-containing hormone replacement therapy containing (HRT).
Because oestrogen is important for regulating the female menstrual cycle, monitoring hormone levels can be used to evaluate ovarian function, particularly the cause of absent periods. Oestrogen levels are monitored through a blood test.
You can check your oestradiol levels with at-home blood test kits from Forth.
MyFORM® Female Hormone Mapping tracks your hormone levels across your menstrual cycle, giving you a unique insight into your unique hormone pattern. This test is for women who are not using hormonal contraception or HRT.
The Female Hormone Imbalance Test analyses 4 key hormones, including oestrogen, to check for hormone imbalances that cause many symptoms. This test is suitable for women who use hormonal contraception or HRT.
Defining a ‘normal’ oestrogen level in women is difficult because there are many confounding factors which can influence a normal level, such as:
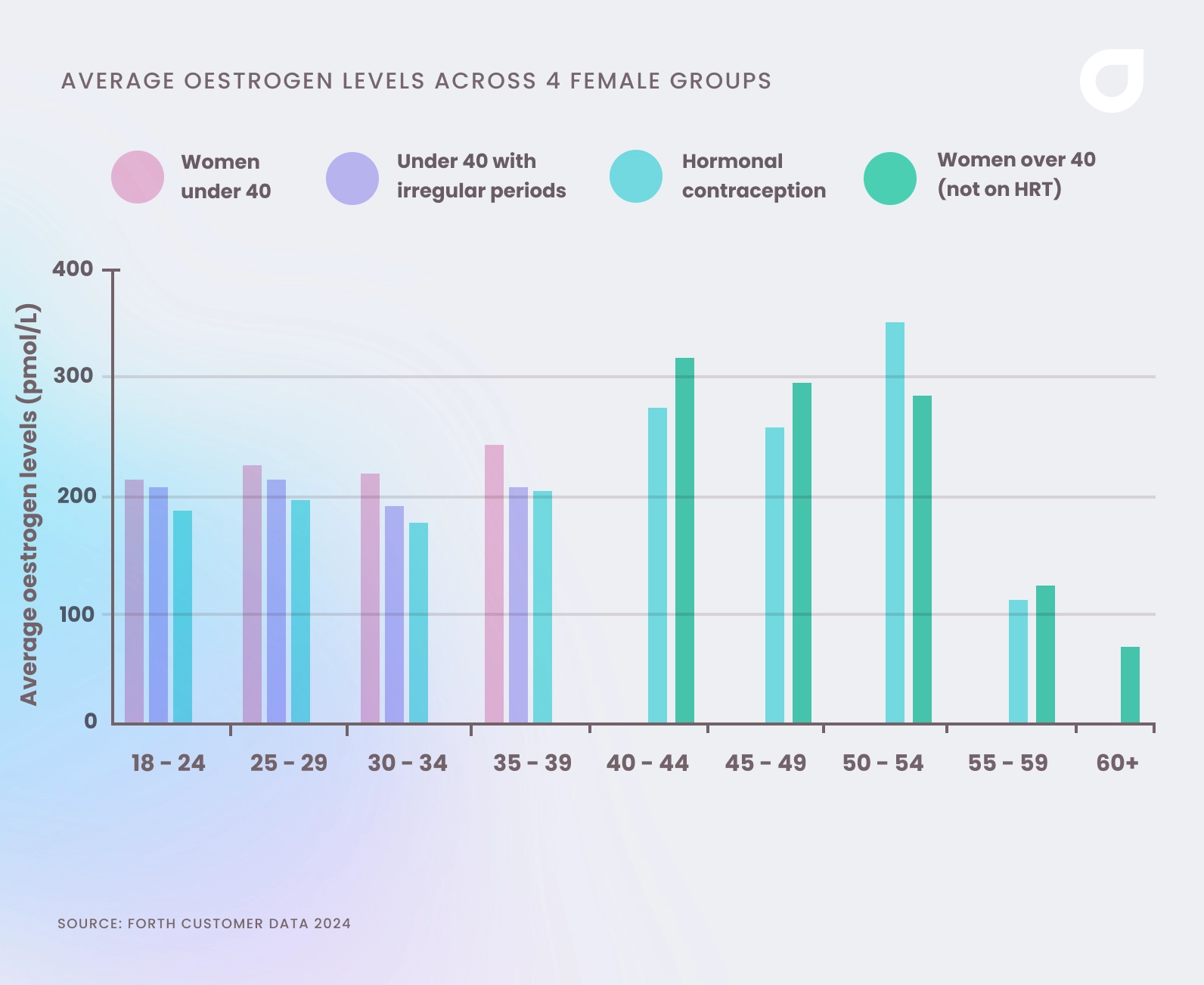
The graph below shows how the average oestrogen level can vary across demographics. In women under 40, oestrogen levels are highest in those in the perimenopause phase, but women who experience irregular periods and those who use hormonal contraception have lower average oestrogen levels.
In the over-40 age group, women who do not take HRT experience a steady decline in oestrogen levels until around 54 before they drop dramatically between 50 and 59.
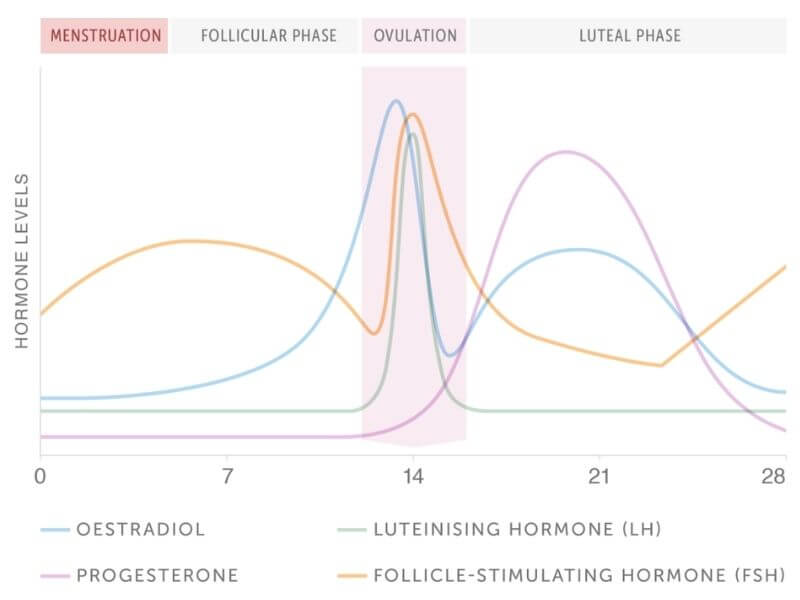
The graphic below shows oestrogen levels rise and fall twice during a normal menstrual cycle. First, they increase during the follicular phase, peaking at the ovulatory stage before dropping dramatically after an egg has been released from an ovary (ovulation).
Oestrogen levels rise again during the luteal phase before falling at the end of the cycle (around day 28). The second rise in oestrogen occurs alongside increasing progesterone, and the corpus luteum produces both hormones. The corpus luteum is a temporary formation of cells that develop after an egg has been released from the ovary. Its main function is to prepare the uterus for pregnancy. Progesterone levels also decline at the end of the menstrual cycle, if pregnancy doesn’t occur and the cycle begins again.
Oestrogen levels naturally fluctuate throughout the menstrual cycle, and although consistently high oestrogen levels may occur naturally, they are usually caused by:
Your body produces too much oestrogen
You’re taking too much maybe in the form of hormonal contraception or hormone replacement therapy
Your body isn’t breaking oestrogen down normally
Several factors contribute to increased oestrogen levels. They are:
There are several reasons why oestradiol levels may rise in men:
| Women | Men |
| Sore breasts Weight gain Headaches Fatigue Low libido Worsening premenstrual syndrome Depression or anxiety Cold hands or feet Heavy periods |
Erectile dysfunction Breast tissue growth (gynecomastia) Infertility |
Hormone imbalances are common, and low oestrogen levels can cause several symptoms, including lighter or non-existent periods. The treatment for low oestrogen will depend on the underlying cause.
Because the ovaries are mainly responsible for producing oestrogen, any condition that affects them can cause low oestrogen levels. Some of the causes include:
The most common cause of declining oestrogen levels is menopause. The body naturally transitions to menopause in your 40s, although this can vary from woman to woman. During this transition period, oestrogen levels can fluctuate from high to low, causing some of the common menopause symptoms. After the menopause, oestrogen levels are very low[10].
Women who have had their ovaries surgically removed will experience menopause and an abrupt start to menopause-related symptoms because of the lack of oestrogen.
Young women who regularly exercise are at a greater risk of developing relative energy deficiency in sports (RED-S). RED-S is a condition characterised by a lack of energy intake which does not compensate for the level of physical activity (energy expenditure)[11].
Alongside a myriad of symptoms, RED-S can cause a hormonal imbalance that suppresses oestrogen levels, leading to missed or in the most severe cases, absent periods (amenorrhoea). RED-S can affect the person’s menstruation and reproductive health, but can also affect their general health and wellbeing.
Anorexia and bulimia are examples of eating disorders that can affect a person’s physical and mental wellbeing[12]. Unhealthy eating practices can also affect fertility, lowering oestrogen levels in women and androgens in men[13].
Conditions such as hyperprolactinemia, where a person has increased levels of the hormone prolactin, can cause low oestrogen levels in women. That’s because prolactin reduces the production of other pituitary hormones, follicle-stimulating hormone (FSH) and luteinising hormone (LH), which act on the ovaries to release oestrogen. A lack of FSH directly affects the secretion of oestrogen from the ovaries[14].
Causes of low oestrogen in men
Low oestrogen levels in men are not usually a cause for concern. However, hormone imbalances may be caused by hypogonadism, a condition where the testes produce little or no hormones, including testosterone and oestrogen.
Hypogonadism in men can be caused by:
| Women | Men |
| Irregular or absent periods Mood swings Hot flashes Breast tenderness Painful sex Depression Fatigue Difficulty concentrating Loss of bone density |
Low libido Bone loss Muscle weakness Fatigue Anxiety Mood changes |
Depending on the cause of a hormonal imbalance, there are several things you can do to help manage your oestrogen levels.
Low oestrogen levels are commonly associated with perimenopause or menopause, so hormone replacement therapy may be an effective way to manage the symptoms. You should discuss HRT with your doctor who will help you decide if it is the right treatment for you.
HRT is available in different preparations and forms, including patches, gels, and tablets. Which type is suitable for you will depend on your blood test results. Your GP will discuss the options with you and which one will be most suitable.
RED-S is defined by low energy availability because of an ongoing calorie deficit, if left untreated it can cause irreparable damage to the body. There are many characteristic warning signs for RED-S in women, the main one being the absence of periods which is a sign of hormone imbalance.
RED-S can be avoided by taking adequate care of your nutrition and balancing it with training and recovery. It is important to pay close attention to your carbohydrate intake when training and your recovery nutrition. You can do this by:
Lifestyle changes can help manage your oestrogen levels. Some of these may help to ‘normalise’ your levels and help you avoid things like hormone replacement therapy. They include:
Phytoestrogens are natural oestrogen-like compounds found in plants and some dairy products. They work by binding to oestrogen receptors and have weak oestrogenic effects in menopausal women.
There are four types of phytoestrogens:
The most commonly studied phytoestrogens are isoflavones and soybeans are the most important source. You’ll need to eat 40 to 70 mg/day to achieve any health effects from phytoestrogens. In the Western world, the average consumption is around 2 mg/day[18].
Other foods that contain phytoestrogens are:
Phytoestrogens may protect against cardiovascular disease and improve heart health, by reducing total cholesterol, blood pressure, and C-reactive protein levels.
Based in the UK, Leanne specialises in writing about health, medicine, nutrition, and fitness.
She has over 5 years of experience in writing about health and lifestyle and has a BSc (hons) Biomedical Science and an MSc Science, Communication and Society.
All these tests include Oestradiol (Oestrogen). Select the test that suits your personal needs.
Certified for quality & security
Emanuele, M. A., Wezeman, F., & Emanuele, N. V. (2002). Alcohol's effects on female reproductive function. Alcohol research & health : the journal of the National Institute on Alcohol Abuse and Alcoholism, 26(4), 274–281.
Razzak, Z. A., Khan, A. A., & Farooqui, S. I. (2019). Effect of aerobic and anaerobic exercise on estrogen level, fat mass, and muscle mass among postmenopausal osteoporotic females. International journal of health sciences, 13(4), 10–16.