
Menopause Test
For women who have reached menopause. Checks key hormones alongside bone health and heart health.
£119
10 mins read
Written by Forth
October 28, 2020
Reviewed by:
Dr Thom Phillips
All women go through menopause, but many don’t really think about until it comes along. It marks a significant point in life for many women, and brings with it a host of symptoms due to changing hormone levels. In this article we take a look at the key hormones that change during the menopause, but first, let’s define what we mean by menopause.
Check your hormones with our at-home Menopause blood test.
Simply, the menopause is when the ovaries no longer respond to the hormonal messages sent from the pituitary gland in the brain. Eventually, this leads to the end of ovulation and the menstrual cycle.
During the build-up to the menopause, known as perimenopause, women’s hormones go through a transformation process. Their levels fluctuate and can alter their physical, mental and emotional wellbeing.
‘I’m feeling hormonal’ can sometimes be bandied about to describe how women feel at a given moment in time, but that feeling can soon become a reality for many women entering the menopausal transition.
There is a plethora of hormones at play in the menopause, all of which have a significant role in bringing about physical and psychological change.
The main hormones are oestrogen, progesterone, and testosterone, but others such as the control hormones follicle-stimulating hormone (FSH) and luteinising hormone (LH) also play a part.
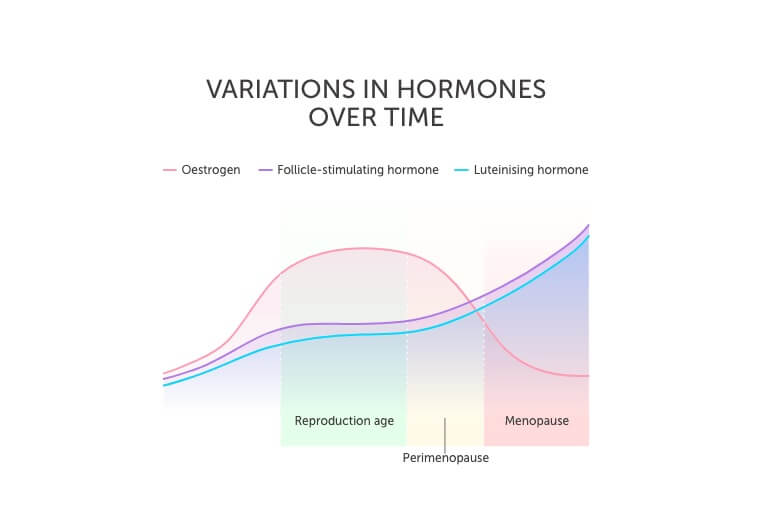
As women enter the perimenopause phase to menopause, the ovaries produce less oestrogen and progesterone. The ovaries become less responsive to the control hormones released by the pituitary gland in the brain – FSH and LH – resulting in higher levels of these control hormones.
We take a look at the three main hormones, oestrogen, progesterone and testosterone, and the roles they play during the menopause.
Oestrogen is mainly produced in the ovaries, but small amounts are also produced in the adrenal glands and is one of the two main sex hormones in women, with the other being progesterone.
The 3 main types of oestrogen in the body:
Oestradiol is the most common type of oestrogen in women of childbearing age, oestriol is the main oestrogen during pregnancy and oestrone is the only oestrogen the body produces after menopause1.
Oestrogen has a role throughout the body and is a key hormone during puberty helping to bring about physical changes and the start of the menstrual cycle1.
Oestrogen helps control the menstrual cycle, is a key hormone in fertility and helping to maintain pregnancy.
Oestrogen levels in women change throughout the month, being highest during the menstrual cycle and lowest during a woman’s period. Oestradiol production enables the development and release of an egg, a process known as ovulation.
Oestrogen is also important in brain function, including mood, as well as contributing to bone and heart health. Oestrogen helps keep cholesterol in control which is why women going through the menopause will have increased cholesterol levels.
As outlined in the chart above, as women age, their ovarian response reduces over time causing fluctuations in oestrogen and progesterone levels during the perimenopause phase until a woman reaches menopause – this is when a woman hasn’t had a period for 12 months.
The normal levels of oestrogen in pre-menopausal women is 45-854 pmol/L. The levels fall to less than 100 pmol/L during the menopause and beyond.
During the normal cycle, the levels of oestrogen and progesterone are in balance with each other. However, as women approach their mid-30s to early 40s, progesterone levels begin to fall, and the ovaries begin to produce less oestrogen.
As a result, women may notice a change in their periods. They may be more or less frequent, last for longer or shorter amounts of time, maybe heavier or lighter. It’s not unusual during perimenopause to have missed periods.
The sharp decline in oestrogen known for causing the symptoms associated with the menopause like hot flushes, vaginal dryness, and memory issues, occurs towards the end of the perimenopause. Here, periods may be lighter and occur less frequently.
It’s important that women going through the menopause look after their bone health as declining oestrogen levels make bones thinner and weaker, increasing the risk of developing osteoporosis.
In the five to seven years following the menopause, women can lose up to one-fifth of their bone density due to the falling levels of oestrogen.
“Bone health in women is very much dependent on oestrogen. Therefore, declining levels will cause deterioration in bone health,” says Dr Nicky Keay, Chief Medical Officer at Forth
Diet and exercise are key to supporting bone health as a woman gets older. Having a diet rich in nutrients key to bone health such as calcium and magnesium as well as taking a vitamin D supplement will help support bone health. As will weight-bearing exercises such as walking and yoga.
“Keeping physically active and loading the skeleton will help. For example, try dancing, walking and strength work. Look at the Royal Osteoporosis Society website where there is a very helpful article ‘Strong, Steady, Straight‘ to combat osteoporosis with exercise”, says Dr Nicky Keay, Chief Medical Officer at Forth
Progesterone is a steroid hormone produced by the body during ovulation. Its main role is to prepare a woman’s body for pregnancy.
Once ovulation has occurred, a small mass of cells called the corpus luteum forms at the location where the ovary released an egg. The corpus luteum starts to produce progesterone. The progesterone prepares the body for pregnancy. Under normal circumstances, progesterone levels peak on day 21 of the menstrual cycle.
If fertilisation of the egg doesn’t occur then the corpus luteum disintegrates, progesterone levels decrease, and a woman has a period.
If an egg is fertilised, the corpus luteum will carry on producing progesterone. A few weeks into pregnancy, the placenta takes over as the main source of progesterone. The placenta produces high amounts of the hormone for the duration of a normal pregnancy.
During the normal menstrual cycle, progesterone works in an opposite manner to oestrogen to keep both hormones in balanced. Oestrogen rises in the first phase of the menstrual cycle to promote the development of an egg, while in the next phase progesterone takes over preparing the body for pregnancy or until the period occurs.
However, during the perimenopause as the ovaries become less responsive levels of oestrogen and progesterone fluctuate, so a woman’s menstrual cycle is less predictable and low progesterone levels can also cause heavier menstrual bleeds2. In addition to changes in a woman’s menstrual cycle, declining progesterone levels can also cause other symptoms such as vaginal dryness. Progesterone helps to thicken the mucus in the cervix but declining levels during the menopause can lead to vaginal dryness.
“Female hormones are not just about oestrogen. The balance of oestrogen to progesterone varies in a set pattern during the menstrual cycle. So, the decrease in both hormones during peri and post menopause, often at different rates and in a variable manner will result in physiological changes. These changes in hormone patterns have physical, mental and psychological impacts” Dr Nicky Keay, Chief Medical Officer at Forth
Menopause symptoms are caused by the declining levels of progesterone, which can no longer balance oestrogen levels, causing oestrogen to become dominant before it, too, declines.
Our innovative perimenopause test, MyFORM™, offers ground-breaking and unparalleled insight into your personal menstrual cycles by mapping how your four key hormones fluctuate throughout your entire menstrual cycle. Combining artificial intelligence with blood analysis and clinical expertise, we are able to provide a score for ovarian responsiveness (FORM score), which along with symptoms, can give confirmation of the onset of perimenopause and the speed of transition towards menopause.
Testosterone is often associated more with men than women and is seen as the ‘male hormone’. However, testosterone plays a key role in a woman’s body too.
Testosterone in women is produced in the ovaries and the adrenal gland and contributes to libido, sexual arousal and orgasm in women as well as maintaining a normal metabolic function, muscle and bone strength, mood, and cognitive function3.
Half of all endogenous testosterone is produced by the ovaries and half is produced by the adrenal glands. Healthy young women produced around 100-400 mcg of testosterone per day, that’s 3 to 4 times the amount of oestrogen produced in the ovaries3.
Unlike progesterone or oestrogen levels which drop dramatically at the time of the menopause, testosterone levels decline slowly as women age. In fact, levels decrease by half between the age of 20 and 40.
Declining testosterone levels can contribute to low libido, changes in cognitive function and mood as well as increasing the risk of developing osteoporosis. Post-menopausal women may also experience acne and an increase in facial hair growth; however, genetics also play a key role in the susceptibility of developing these problems3.
Women will experience hormone imbalance as they enter and transition through to menopause due to declining oestrogen, progesterone and testosterone levels and a rise in control hormones FSH and LH.
These hormone changes will impact a woman’s physical and mental health to varying degrees during the perimenopause with a range of symptoms experienced.
So, what can be done to help ease the symptoms due to fluctuating hormones during the menopause?
As Dr Nicky Keay explains, it’s all about educating yourself on the changes that are going to be taking place during the menopause and the options available to manage symptoms.
“Empowering yourself with information is key when it comes to the menopause. In the first instance knowing that the symptoms you are experiencing is due to changing hormones gives you understanding of what’s going on in your body. This provides an opportunity to consider your options, whether it’s changes in lifestyle or deciding to go on HRT.”
HRT is used to help women manage their symptoms during the menopause by replacing oestrogen and progesterone. Dr Keay adds, “despite recent reports, HRT is safe in those for whom HRT is not contraindicated. Although there is a slight increase in the risk of breast cancer, it is nowhere near as high as the risk associated with suboptimal lifestyle factors such as being overweight, smoking and drinking excessive alcohol. As with any medication risk/benefits must be weighed up for the individual. For many HRT improves quality of life.”
For further reading, we’ve created a comprehensive Guide To The Menopause, as well as guides on HRT and menopause symptoms.
Understanding the menopause and the changes that will take place is key to managing this natural part of life.

Our Menopause Health Blood Test is designed for women who have already reached menopause (12+ months without a period). Your sample is analysed by an accredited NHS laboratory in the UK, ensuring reliable and accurate results. This test helps you monitor key female hormone levels, including oestrogen and progesterone, as well as important biomarkers for bone strength and heart health – two areas of increased risk after menopause. It’s also an effective way to assess how well your HRT is working, helping you make informed decisions about your treatment and overall well-being.

For women who have reached menopause. Checks key hormones alongside bone health and heart health.
£119
Thom works in NHS general practice and has a decade of experience working in both male and female elite sport. He has a background in exercise physiology and has published research into fatigue biomarkers.

Dr Thom Phillips
Chief Medical Officer
Like this article? Here are some more based on similar topics.